Vitamin D: A Comprehensive Guide
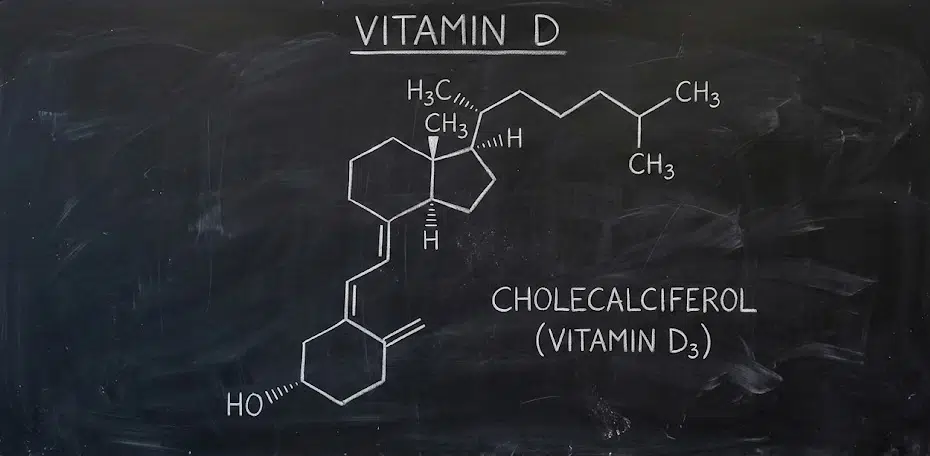
Vitamin D is a fat-soluble vitamin that functions as both a nutrient and a hormone in the human body. Unlike most vitamins, your body can synthesize vitamin D when skin is exposed to ultraviolet B (UVB) radiation from sunlight. This unique characteristic has led researchers to classify it as a secosteroid rather than a traditional vitamin.
The two main forms relevant to human health are vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol). Both must undergo two hydroxylation reactions—first in the liver, then in the kidneys—to become calcitriol, the biologically active form that regulates calcium absorption, bone metabolism, immune function, and gene expression in cells throughout the body.
Vitamin D deficiency affects an estimated 1 billion people worldwide.1Holick MF. Vitamin D deficiency. N Engl J Med. 2007;357(3):266-281. Insufficient levels have been linked to bone diseases, increased infection risk, autoimmune conditions, cardiovascular disease, and certain cancers, though the strength of evidence varies across these associations.
Understanding Vitamin D Forms and Metabolism
The term “vitamin D” encompasses several related compounds that your body converts through a series of chemical transformations.
Vitamin D2 vs. Vitamin D3
Vitamin D2 (ergocalciferol):
- Produced by plants, mushrooms, and yeast when exposed to UV light
- Derived from ergosterol
- Less stable than D3
- May be less effective at raising blood levels of 25(OH)D
Vitamin D3 (cholecalciferol):
- Synthesized in human skin from 7-dehydrocholesterol when exposed to UVB radiation
- Found in animal-based foods (fatty fish, egg yolks, liver)
- More potent than D2 at increasing serum 25(OH)D concentrations
- The form used in most supplements
Multiple studies show vitamin D3 raises and maintains 25(OH)D levels more effectively than equivalent doses of vitamin D2.2Tripkovic L, Lambert H, Hart K, et al. Comparison of vitamin D2 and vitamin D3 supplementation in raising serum 25-hydroxyvitamin D status: a systematic review and meta-analysis. Am J Clin Nutr. 2012;95(6):1357-1364. A meta-analysis found that vitamin D3 was approximately 87% more effective than D2 at raising and maintaining 25(OH)D concentrations.
The Conversion Pathway
Vitamin D undergoes two hydroxylation steps before becoming active:
- First hydroxylation (liver): Vitamin D → 25-hydroxyvitamin D [25(OH)D, calcidiol]
- This is the major circulating form
- Blood tests measure 25(OH)D to assess vitamin D status
- Half-life of approximately 2-3 weeks
- Second hydroxylation (kidneys and other tissues): 25(OH)D → 1,25-dihydroxyvitamin D [1,25(OH)2D, calcitriol]
- This is the biologically active hormone
- Half-life of only 4-6 hours
- Tightly regulated by parathyroid hormone (PTH), calcium, and phosphate levels
The kidney enzyme 1α-hydroxylase catalyzes the second conversion. However, many other tissues—including immune cells, prostate, breast, colon, and skin—also express this enzyme and can produce calcitriol locally for autocrine and paracrine functions.3Bikle DD, Christakos S. New aspects of vitamin D metabolism and action – addressing the skin as source and target. Nat Rev Endocrinol. 2020;16(4):234-252.
Regulation and Feedback
Your body regulates vitamin D metabolism through several feedback mechanisms:
- Fibroblast growth factor 23 (FGF23) inhibits 1α-hydroxylase and stimulates 24-hydroxylase, which degrades both 25(OH)D and calcitriol
- Parathyroid hormone (PTH) increases 1α-hydroxylase activity when calcium is low
- High calcium levels suppress PTH and reduce calcitriol production
- Calcitriol itself induces 24-hydroxylase, creating a negative feedback loop
This complex regulation prevents excessive calcitriol production even when vitamin D intake or synthesis is high, which is why vitamin D toxicity from sun exposure alone is virtually impossible.
Mechanisms of Action
Calcitriol exerts its effects through both genomic and non-genomic pathways.
Genomic Actions via Vitamin D Receptor
The vitamin D receptor (VDR) is a nuclear receptor found in nearly every tissue in the body. When calcitriol binds to VDR, the complex:
- Heterodimerizes with the retinoid X receptor (RXR)
- Binds to vitamin D response elements (VDREs) in DNA
- Recruits coactivator proteins
- Modulates transcription of hundreds of genes
Genes regulated by VDR include those involved in:
- Calcium and phosphate transport (TRPV6, calbindin, PMCA1b)
- Bone formation and remodeling (osteocalcin, osteopontin, RANKL)
- Cell proliferation and differentiation (p21, p27)
- Immune function (cathelicidin, defensins)
- Inflammatory responses (multiple cytokines)
Research suggests VDR influences expression of 3-5% of the human genome.4Haussler MR, Whitfield GK, Kaneko I, et al. Molecular mechanisms of vitamin D action. Calcif Tissue Int. 2013;92(2):77-98.
Non-Genomic Actions
Calcitriol also triggers rapid cellular responses (within seconds to minutes) through membrane-associated receptors and signaling cascades:
- Opening of voltage-gated calcium channels
- Activation of protein kinase C
- Stimulation of MAP kinase pathways
- Modulation of intracellular calcium concentrations
These quick responses occur too rapidly to involve gene transcription and instead affect immediate cellular functions like muscle contraction, insulin secretion, and inflammatory responses.
Calcium Homeostasis
Vitamin D’s classical function is maintaining calcium and phosphate balance:
In the intestine: Calcitriol increases expression of calcium transport proteins (TRPV6, calbindin-D9k), enhancing calcium absorption from 10-15% (when deficient) to 30-40% (when replete).5Fleet JC, Schoch RD. Molecular mechanisms for regulation of intestinal calcium absorption by vitamin D and other factors. Crit Rev Clin Lab Sci. 2010;47(4):181-195.
In the kidneys: Vitamin D promotes calcium reabsorption in the distal tubules, reducing urinary calcium loss.
In bone: The relationship is complex. Adequate vitamin D is required for proper bone mineralization, but calcitriol also stimulates osteoclast formation (bone resorption) when working with PTH to raise blood calcium. The net effect depends on overall calcium status.
Immune System Modulation
Immune cells express both VDR and 1α-hydroxylase, allowing them to respond to and produce calcitriol locally. Vitamin D influences both innate and adaptive immunity:
Innate immunity:
- Increases production of antimicrobial peptides (cathelicidin, β-defensins)
- Enhances chemotaxis and phagocytic capacity of macrophages
- Promotes autophagy in infected cells
Adaptive immunity:
- Inhibits T cell proliferation and cytokine production
- Promotes regulatory T cells (Tregs)
- Suppresses B cell proliferation and antibody production
- Shifts immune response from Th1 (pro-inflammatory) toward Th2 (anti-inflammatory)
These immunomodulatory effects explain vitamin D’s role in both infection resistance and autoimmune disease.6Aranow C. Vitamin D and the immune system. J Investig Med. 2011;59(6):881-886.
Vitamin D Status and Testing
Measuring Vitamin D Levels
Clinicians measure 25(OH)D rather than calcitriol because:
- 25(OH)D has a longer half-life (2-3 weeks vs. 4-6 hours)
- Circulates at concentrations 1000-fold higher than calcitriol
- Better reflects vitamin D stores
- Calcitriol can appear normal even in deficiency due to secondary hyperparathyroidism
Two assays exist for measuring 25(OH)D:
- Liquid chromatography-tandem mass spectrometry (LC-MS/MS): Gold standard, measures D2 and D3 separately
- Immunoassays: More widely available but can vary between laboratories
Interpreting Results
No universal consensus exists on optimal 25(OH)D levels, but most expert groups use these categories:
- Deficiency: <20 ng/mL (<50 nmol/L)
- Insufficiency: 20-29 ng/mL (50-74 nmol/L)
- Sufficiency: 30-50 ng/mL (75-125 nmol/L)
- High normal: 50-100 ng/mL (125-250 nmol/L)
- Excess/Toxicity risk: >100 ng/mL (>250 nmol/L)
The Institute of Medicine (now National Academy of Medicine) considers 20 ng/mL adequate for bone health in the general population.7Institute of Medicine (US) Committee to Review Dietary Reference Intakes for Vitamin D and Calcium. Dietary Reference Intakes for Calcium and Vitamin D. Washington (DC): National Academies Press; 2011.
The Endocrine Society recommends 30 ng/mL as the minimum for optimal health, acknowledging that extraskeletal benefits may require higher levels.8Holick MF, Binkley NC, Bischoff-Ferrari HA, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96(7):1911-1930.
Factors Affecting Vitamin D Status
Geographic and seasonal variation: UVB radiation varies by latitude, season, and time of day. In locations above 37°N latitude (roughly San Francisco, Virginia, Athens), skin cannot produce vitamin D from November through February.9Webb AR, Kline L, Holick MF. Influence of season and latitude on the cutaneous synthesis of vitamin D3: exposure to winter sunlight in Boston and Edmonton will not promote vitamin D3 synthesis in human skin. J Clin Endocrinol Metab. 1988;67(2):373-378.
Skin pigmentation: Melanin absorbs UVB radiation before it reaches 7-dehydrocholesterol. Dark-skinned individuals require 3-5 times longer sun exposure than light-skinned individuals to produce equivalent vitamin D.10Clemens TL, Adams JS, Henderson SL, Holick MF. Increased skin pigment reduces the capacity of skin to synthesise vitamin D3. Lancet. 1982;1(8263):74-76.
Age: Aging reduces skin’s capacity to produce vitamin D. A 70-year-old has more than a twofold reduction in previtamin D3 synthesis compared to young adults under identical sun exposure conditions.11MacLaughlin J, Holick MF. Aging decreases the capacity of human skin to produce vitamin D3. J Clin Invest. 1985;76(4):1536-1538.
Obesity: Vitamin D is sequestered in adipose tissue, reducing its bioavailability. Obese individuals (BMI >30) may require 2-3 times higher intake to achieve the same 25(OH)D levels as normal-weight individuals.12Wortsman J, Matsuoka LY, Chen TC, Lu Z, Holick MF. Decreased bioavailability of vitamin D in obesity. Am J Clin Nutr. 2000;72(3):690-693.
Sunscreen use: SPF 30 reduces vitamin D synthesis by approximately 95-98%.13Matsuoka LY, Ide L, Wortsman J, MacLaughlin JA, Holick MF. Sunscreens suppress cutaneous vitamin D3 synthesis. J Clin Endocrinol Metab. 1987;64(6):1165-1168. However, real-world sunscreen application is typically incomplete, allowing some vitamin D production.
Medical conditions:
- Malabsorption disorders (celiac disease, Crohn’s disease, cystic fibrosis)
- Kidney disease (impairs 1α-hydroxylase)
- Liver disease (impairs 25-hydroxylation)
- Hyperparathyroidism
- Certain medications (see Drug Interactions section)
Clinical Evidence for Health Benefits
Research on vitamin D extends beyond bone health to numerous other conditions. The quality of evidence varies considerably.
Bone Health and Fracture Prevention
Vitamin D’s role in bone health is well-established and uncontroversial.
Rickets and osteomalacia: Severe vitamin D deficiency causes rickets in children (characterized by soft, weak bones and skeletal deformities) and osteomalacia in adults (bone pain, muscle weakness, increased fracture risk). These conditions are definitively treated with vitamin D supplementation.14Thacher TD, Clarke BL. Vitamin D insufficiency. Mayo Clin Proc. 2011;86(1):50-60.
Osteoporosis and fractures: The relationship between vitamin D and fracture risk is complex. A 2018 meta-analysis of 81 randomized controlled trials found that vitamin D supplementation with calcium reduced hip fracture risk by 16% and any fracture by 6% compared to placebo or no treatment.15Yao P, Bennett D, Mafham M, et al. Vitamin D and calcium for the prevention of fracture: a systematic review and meta-analysis. JAMA Netw Open. 2019;2(12):e1917789.
However, vitamin D alone (without calcium) showed inconsistent results. Benefits appeared strongest in:
- Individuals with baseline 25(OH)D <20 ng/mL
- Institutionalized elderly populations
- Those taking doses ≥800 IU daily
- When combined with adequate calcium intake
A 2020 trial (VITAL study) found that 2000 IU daily vitamin D did not reduce fracture incidence in generally healthy adults with mean baseline 25(OH)D of 30.7 ng/mL.16LeBoff MS, Chou SH, Ratliff KA, et al. Supplemental vitamin D and incident fractures in midlife and older adults. N Engl J Med. 2022;387(4):299-309. This suggests benefits may be limited to those who are truly deficient.
Immune Function and Infection Risk
Respiratory infections: Observational studies consistently link low vitamin D status with increased respiratory infection rates. A 2017 meta-analysis of 25 randomized controlled trials (total 10,933 participants) found that vitamin D supplementation reduced the risk of acute respiratory infections by 12% overall.17Martineau AR, Jolliffe DA, Hooper RL, et al. Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ. 2017;356:i6583.
The protective effect was stronger among:
- Those with baseline 25(OH)D <10 ng/mL (number needed to treat = 4)
- Daily or weekly dosing (vs. large bolus doses)
- Those not receiving bolus doses ≥30,000 IU
COVID-19: Early in the pandemic, low vitamin D status was associated with COVID-19 infection risk and severity in observational studies. However, randomized trials have produced mixed results. A 2022 meta-analysis of 17 trials found no significant benefit of vitamin D supplementation on COVID-19 outcomes in hospitalized patients.18Pal R, Banerjee M, Bhadada SK, Shetty AJ, Singh B, Vyas A. Vitamin D supplementation and clinical outcomes in COVID-19: a systematic review and meta-analysis. J Endocrinol Invest. 2022;45(1):53-68. Prevention trials in the general population showed similarly inconsistent effects.
Autoimmune diseases: Vitamin D’s immunomodulatory properties have prompted investigation in autoimmune conditions:
Multiple sclerosis: Observational studies show strong inverse associations between vitamin D status and MS risk. Each 20 ng/mL increase in 25(OH)D correlates with approximately 40% lower MS risk.19Munger KL, Levin LI, Hollis BW, Howard NS, Ascherio A. Serum 25-hydroxyvitamin D levels and risk of multiple sclerosis. JAMA. 2006;296(23):2832-2838. However, supplementation trials in established MS have not shown consistent benefits in disease progression.
Type 1 diabetes: Vitamin D supplementation in infancy has been associated with reduced T1D risk in observational studies, but randomized trials are lacking due to ethical and practical constraints.
Rheumatoid arthritis, lupus, inflammatory bowel disease: Limited trial data exists, with most evidence coming from observational studies showing associations between low vitamin D and disease activity.
Cardiovascular Health
The relationship between vitamin D and cardiovascular disease remains uncertain despite extensive research.
Observational studies consistently show that individuals with low 25(OH)D levels have higher rates of:
- Hypertension
- Coronary artery disease
- Heart failure
- Stroke
- Cardiovascular mortality
However, causality remains unproven. The VITAL trial, a large randomized controlled trial of 2000 IU daily vitamin D in 25,871 adults followed for 5.3 years, found no reduction in major cardiovascular events (myocardial infarction, stroke, or cardiovascular death) compared to placebo.20Manson JE, Cook NR, Lee IM, et al. Vitamin D supplements and prevention of cancer and cardiovascular disease. N Engl J Med. 2019;380(1):33-44.
The trial enrolled relatively healthy participants with adequate baseline vitamin D status (median 30.8 ng/mL), potentially explaining the null results. Whether supplementation benefits those with true deficiency or established cardiovascular disease remains unclear.
Cancer Prevention
Mechanistic studies show vitamin D can inhibit cancer cell proliferation, promote differentiation, induce apoptosis, and reduce angiogenesis and metastasis in laboratory models. Epidemiological data has produced mixed results.
Colorectal cancer: The strongest evidence exists for colorectal cancer. A 2019 meta-analysis found that each 4 ng/mL increase in 25(OH)D was associated with 19% lower colorectal cancer risk.21McCullough ML, Zoltick ES, Weinstein SJ, et al. Circulating vitamin D and colorectal cancer risk: an international pooling project of 17 cohorts. J Natl Cancer Inst. 2019;111(2):158-169.
The VITAL trial found no significant reduction in total cancer incidence with 2000 IU daily vitamin D. However, secondary analyses suggested possible reductions in cancer mortality and metastatic or fatal cancer.22Chandler PD, Chen WY, Ajala ON, et al. Effect of vitamin D3 supplements on development of advanced cancer: a secondary analysis of the VITAL randomized clinical trial. JAMA Netw Open. 2020;3(11):e2025850.
Other cancers: Evidence for breast, prostate, lung, and other cancers is less consistent. Some observational studies show inverse associations, but randomized trials have not confirmed protective effects.
Mood and Mental Health
Depression: Cross-sectional studies often find lower vitamin D levels in individuals with depression. A 2020 meta-analysis of randomized controlled trials found that vitamin D supplementation reduced depression symptoms compared to placebo, with a small-to-moderate effect size.23Vellekkatt F, Menon V. Efficacy of vitamin D supplementation in major depression: A meta-analysis of randomized controlled trials. J Postgrad Med. 2019;65(2):74-80.
Effects appeared stronger in:
- Those with clinical depression (vs. depressive symptoms in non-clinical populations)
- Those with baseline vitamin D deficiency
- Studies using adequate doses (≥2000 IU daily)
Cognitive function: Observational studies link low vitamin D to cognitive decline and dementia risk. However, supplementation trials have not shown benefits in preventing cognitive decline in older adults without baseline deficiency.24Pettersen JA. Does high dose vitamin D supplementation enhance cognition?: A randomized trial in healthy adults. Exp Gerontol. 2017;90:90-97.
Muscle Function and Falls
Vitamin D receptors are expressed in skeletal muscle, and deficiency is associated with muscle weakness, particularly in the elderly.
A 2018 meta-analysis found that vitamin D supplementation reduced fall risk by 12% in older adults.25Zhao JG, Zeng XT, Wang J, Liu L. Association between calcium or vitamin D supplementation and fracture incidence in community-dwelling older adults: a systematic review and meta-analysis. JAMA. 2017;318(24):2466-2482. Benefits were most apparent when:
- Baseline 25(OH)D was <20 ng/mL
- Doses of 700-1000 IU daily were used
- Calcium was also supplemented
Metabolic Health
Type 2 diabetes: Observational studies show inverse associations between vitamin D status and diabetes risk. Several randomized trials have tested whether supplementation prevents diabetes in high-risk individuals.
A 2019 trial (D2d study) in 2,423 adults with prediabetes found that 4000 IU daily vitamin D reduced diabetes incidence by 12% compared to placebo, though this did not reach statistical significance (p=0.12).26Pittas AG, Dawson-Hughes B, Sheehan P, et al. Vitamin D supplementation and prevention of type 2 diabetes. N Engl J Med. 2019;381(6):520-530. Post-hoc analyses suggested benefits were concentrated in those with baseline 25(OH)D <12 ng/mL.
Weight and body composition: Despite biological plausibility (vitamin D deficiency in obesity, VDR in adipocytes), supplementation trials have not shown consistent benefits for weight loss or body composition changes in obese individuals.27Mallard SR, Howe AS, Houghton LA. Vitamin D status and weight loss: a systematic review and meta-analysis of randomized and nonrandomized controlled weight-loss trials. Am J Clin Nutr. 2016;104(4):1151-1159.
Dietary Sources and Sun Exposure
Food Sources
Few foods naturally contain significant vitamin D:
High sources (per 3.5 oz/100g):
- Cod liver oil: 10,000 IU (250 μg)
- Salmon, wild: 600-1000 IU (15-25 μg)
- Salmon, farmed: 100-250 IU (2.5-6.25 μg)
- Mackerel: 360 IU (9 μg)
- Sardines: 270 IU (6.75 μg)
- Tuna, canned: 236 IU (5.9 μg)
Moderate sources:
- Egg yolk: 37 IU (0.9 μg) per large egg
- Beef liver: 42 IU (1.05 μg)
- Cheese: 24 IU (0.6 μg)
- Mushrooms, UV-exposed: Variable, 200-800 IU (5-20 μg)
Fortified foods:
- Milk (fortified): 100 IU (2.5 μg) per cup
- Orange juice (fortified): 100 IU (2.5 μg) per cup
- Cereals (fortified): 40-100 IU (1-2.5 μg) per serving
- Yogurt (fortified): 80 IU (2 μg) per 6 oz
For most people, dietary intake alone is insufficient to maintain optimal vitamin D status without supplementation or sun exposure.
Sun Exposure Guidelines
UVB radiation triggers vitamin D synthesis when it penetrates the skin. The amount produced depends on:
- UV index: Higher at lower latitudes, during summer, midday (10 AM – 3 PM)
- Skin surface area exposed: More skin = more production
- Skin tone: Lighter skin produces vitamin D faster
- Duration: Synthesis peaks then declines (further exposure doesn’t help)
General guidance: Exposing 25% of body surface area (arms and legs) to midday sun for 10-30 minutes several times per week can produce adequate vitamin D in light-skinned individuals. Darker-skinned individuals may need 3-6 times longer exposure.
Practical limitations:
- Balancing vitamin D production against skin cancer risk
- UVB doesn’t penetrate glass
- Seasonal and geographic constraints
- Pollution and cloud cover reduce UVB
- Lifestyle factors (indoor occupations, clothing)
Most dermatologists and cancer organizations prioritize sun protection over vitamin D production, recommending supplementation instead.
Supplementation Protocols
Recommended Daily Allowances
The Institute of Medicine established these Recommended Dietary Allowances (RDAs):
- Infants 0-12 months: 400 IU (10 μg)
- Children 1-18 years: 600 IU (15 μg)
- Adults 19-70 years: 600 IU (15 μg)
- Adults >70 years: 800 IU (20 μg)
- Pregnancy and lactation: 600 IU (15 μg)
Tolerable Upper Intake Level (UL):
- Infants 0-6 months: 1000 IU (25 μg)
- Infants 7-12 months: 1500 IU (38 μg)
- Children 1-3 years: 2500 IU (63 μg)
- Children 4-8 years: 3000 IU (75 μg)
- Ages 9+: 4000 IU (100 μg)
These recommendations assume minimal sun exposure and target 25(OH)D levels of approximately 20 ng/mL.
Therapeutic Dosing
For individuals with documented deficiency (<20 ng/mL), higher initial doses may be warranted:
Correction protocols:
- Severe deficiency (<10 ng/mL): 50,000 IU weekly for 8-12 weeks, then maintenance
- Moderate deficiency (10-20 ng/mL): 50,000 IU weekly for 4-8 weeks, or 4000-6000 IU daily
- Insufficiency (20-30 ng/mL): 2000-4000 IU daily
Maintenance dosing after correction:
- 1000-2000 IU daily for most adults
- 2000-4000 IU daily for those with risk factors (obesity, dark skin, limited sun exposure, malabsorption)
The Endocrine Society suggests maintaining 25(OH)D at 30-50 ng/mL for optimal health benefits, which typically requires 1500-2000 IU daily in adults.28Holick MF, Binkley NC, Bischoff-Ferrari HA, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96(7):1911-1930.
Dosing Schedules
Daily dosing: Most research supports daily supplementation as superior to weekly or monthly boluses. Daily dosing produces more stable 25(OH)D levels and appears more effective for non-skeletal outcomes.
Weekly dosing: Can be effective for convenience. Example: 7000 IU once weekly is approximately equivalent to 1000 IU daily.
Monthly or bolus dosing: Large infrequent doses (50,000-100,000 IU monthly or less frequently) produce saw-tooth blood level patterns and have shown inferior results for falls, fractures, and infections compared to daily dosing.29Martineau AR, Jolliffe DA, Hooper RL, et al. Vitamin D supplementation to prevent acute respiratory tract infections: systematic review and meta-analysis of individual participant data. BMJ. 2017;356:i6583.
Special Populations
Infants: Exclusively breastfed infants should receive 400 IU daily from birth, as breast milk contains minimal vitamin D (typically 20-60 IU/L even in replete mothers).
Pregnant women: Pregnancy does not increase vitamin D requirements, but many pregnant women are deficient. Some experts recommend 1000-2000 IU daily, though routine screening during pregnancy remains debated.
Obese individuals: May require 2-3 times the standard dose to achieve target 25(OH)D levels due to sequestration in adipose tissue.
Malabsorption conditions: Individuals with celiac disease, Crohn’s disease, cystic fibrosis, or status post-bariatric surgery often require higher doses (3000-6000 IU daily or more) and should have levels monitored.
Bioavailability and Absorption
Vitamin D is fat-soluble, and absorption follows the same pathway as dietary fats.
Factors Affecting Absorption
Dietary fat: Taking vitamin D supplements with a meal containing fat increases absorption by 32-56% compared to fasting.30Dawson-Hughes B, Harris SS, Lichtenstein AH, Dolnikowski G, Palermo NJ, Rasmussen H. Dietary fat increases vitamin D-3 absorption. J Acad Nutr Diet. 2015;115(2):225-230. Even a small amount of fat (11g) is sufficient to enhance absorption significantly.
Supplement formulation:
- Oil-based softgels: Generally well-absorbed
- Dry tablets/capsules: Absorption depends on gastric pH and bile acid availability
- Emulsified or micellized forms: May offer improved absorption but limited comparative data exists
- Liposomal formulations: Theoretical advantages but clinical superiority not established
Magnesium status: Magnesium is a cofactor for enzymes that activate vitamin D. Deficiency may impair conversion of vitamin D to active forms, though this relationship is complex and not fully understood.31Uwitonze AM, Razzaque MS. Role of magnesium in vitamin D activation and function. J Am Osteopath Assoc. 2018;118(3):181-189.
For more information on optimizing supplement absorption, see our article on supplement bioavailability.
Time to Effect
After supplementation begins:
- 25(OH)D levels begin rising within days
- Peak concentration occurs at 3-4 months with daily dosing
- Steady state is reached at approximately 3 months
- After stopping supplementation, levels decline with a half-life of 2-3 weeks
This means testing should occur no sooner than 3 months after starting supplementation or changing doses to assess true steady-state levels.
Toxicity and Safety Concerns
Vitamin D toxicity (hypervitaminosis D) is rare but potentially serious.
Mechanisms of Toxicity
Excessive vitamin D causes:
- Hypercalcemia (elevated blood calcium)
- Hypercalciuria (elevated urinary calcium)
- Calcium deposition in soft tissues (kidneys, blood vessels, heart, lungs)
These effects result from excessive calcitriol production overwhelming normal regulatory mechanisms.
Toxicity Threshold
Vitamin D toxicity typically requires sustained intake of doses far exceeding the UL:
- Single doses up to 300,000 IU do not cause toxicity in adults
- Chronic intake of 10,000-40,000 IU daily for months can produce toxicity
- Most reported cases involve intake >40,000 IU daily or manufacturing errors in supplements
Toxicity is virtually never caused by sun exposure, as skin production is self-limiting (excess previtamin D degrades into inactive metabolites).
Symptoms of Toxicity
Early symptoms (related to hypercalcemia):
- Nausea and vomiting
- Poor appetite
- Constipation
- Weakness and fatigue
- Confusion
- Excessive thirst and urination
Late symptoms:
- Kidney stones
- Kidney damage
- Bone pain
- Cardiac arrhythmias
- Nephrocalcinosis (calcium deposits in kidneys)
Safety of High-Dose Supplementation
4000 IU daily (UL): Extensive research shows this dose is safe for long-term use in adults without causing hypercalcemia or adverse effects.32Hathcock JN, Shao A, Vieth R, Heaney R. Risk assessment for vitamin D. Am J Clin Nutr. 2007;85(1):6-18.
10,000 IU daily: Several studies have used this dose for up to 5 months without toxicity, though 25(OH)D levels should be monitored. Not recommended for routine use without medical supervision.
>10,000 IU daily: Should only be used under medical supervision with regular monitoring of 25(OH)D, calcium, and kidney function.
Hypercalcemia Risk Factors
Certain conditions increase susceptibility to vitamin D-induced hypercalcemia:
- Primary hyperparathyroidism
- Granulomatous diseases (sarcoidosis, tuberculosis)
- Some lymphomas
- Immobilization
- Thiazide diuretic use
- Kidney disease (impaired calcium excretion)
Drug and Nutrient Interactions
Vitamin D interacts with numerous medications and other nutrients.
Medications Reducing Vitamin D Levels
Corticosteroids: Prednisone and other glucocorticoids reduce calcium absorption, increase calcium excretion, and impair vitamin D metabolism. Long-term corticosteroid users often require vitamin D supplementation to prevent bone loss.
Anticonvulsants: Phenytoin, phenobarbital, and carbamazepine induce CYP24A1, accelerating vitamin D catabolism. Patients on chronic anticonvulsant therapy may need 2-4 times the standard vitamin D dose.
Antiretrovirals: Some HIV medications (efavirenz, certain protease inhibitors) reduce 25(OH)D levels through hepatic enzyme induction.
Orlistat: This weight-loss medication inhibits fat absorption, thereby reducing absorption of fat-soluble vitamins including vitamin D. Vitamin D should be taken at least 2 hours before or after orlistat.
Cholestyramine and colestipol: These bile acid sequestrants reduce vitamin D absorption. Separate administration by 4-6 hours.
Medications Affected by Vitamin D
Thiazide diuretics: The combination of vitamin D and thiazides (which reduce urinary calcium excretion) can lead to hypercalcemia, particularly in elderly individuals. Monitor calcium levels if using both.
Digoxin: Hypercalcemia from vitamin D toxicity can increase risk of cardiac arrhythmias in patients taking digoxin.
Hydroxychloroquine: This antimalarial/immunosuppressant drug can increase calcitriol levels, potentially leading to hypercalcemia when combined with vitamin D supplementation.
Nutrient Interactions
Calcium: Vitamin D increases calcium absorption. While this is beneficial up to a point, excessive calcium intake (>2000-2500 mg daily) combined with high-dose vitamin D could theoretically increase soft tissue calcification risk. See our general Nutrition article for more on calcium balance.
Magnesium: Required for vitamin D metabolism. Magnesium deficiency may blunt the response to vitamin D supplementation. Some practitioners recommend combining vitamin D with magnesium, particularly in deficient individuals. See our comparison of Magnesium Glycinate vs Magnesium Citrate vs Magnesium Oxide for choosing magnesium forms.
Vitamin K2: Works synergistically with vitamin D to regulate calcium metabolism. Vitamin D increases calcium absorption, while vitamin K2 activates proteins (osteocalcin, matrix Gla protein) that direct calcium to bones and away from soft tissues. Some researchers recommend combining D and K2, especially at higher vitamin D doses.
Vitamin A: High-dose vitamin A (>10,000 IU retinol daily) may interfere with vitamin D action and contribute to bone loss. This typically occurs only with high-dose retinol supplementation, not from food sources or beta-carotene.
Choosing a Vitamin D Supplement
D2 vs. D3 Supplements
Based on research showing superior potency, vitamin D3 (cholecalciferol) is generally preferred over D2 (ergocalciferol) for supplementation. The exception is for strict vegans who may prefer plant-derived D2 or lichen-sourced vegan D3 (now available).
Dosage Forms
Softgels/liquid:
- Generally well-absorbed
- Often contain oil to enhance absorption
- Easy to swallow
- Suitable for those who have difficulty with tablets
Tablets/capsules:
- Convenient
- Long shelf life
- Should be taken with fat-containing food
- Vary in dissolution rates
Liquid drops:
- Precise dose adjustment
- Good for children or those with swallowing difficulties
- Allows very high doses in small volume
- May have shorter shelf life once opened
Gummies:
- Palatability advantage
- Often contain added sugars
- May have lower potency than stated due to degradation
- Absorption similar to other forms when taken with food
Prescription formulations: High-dose prescription vitamin D (ergocalciferol 50,000 IU capsules) is vitamin D2. Over-the-counter D3 at equivalent doses (50,000 IU) is available and generally preferred.
Quality Considerations
Third-party testing: Look for products verified by:
These organizations test for:
- Potency accuracy
- Contaminant screening (heavy metals, microbes)
- Disintegration/dissolution
- Label accuracy
For more details on certification standards, see our Supplement Certifications Compared article and individual certification guides for NSF, USP, Informed Choice, BSCG, and International Supplement Certification.
Stability and storage: Vitamin D is relatively stable. Store in cool, dry place away from light. Oil-based preparations maintain potency better than dry forms.
Combination Products
Calcium + D: Common combination for bone health. Convenient but may not provide optimal doses of each nutrient individually. Many people need more vitamin D than the fixed ratio provides.
D + K2: Common combination based on synergistic calcium metabolism effects. Typical ratios vary (100-200 μg K2 per 1000-5000 IU D3). Limited clinical data on optimal ratios.
Multivitamins: Often contain 400-1000 IU vitamin D. Insufficient for individuals with deficiency or increased needs. May serve as baseline intake but rarely adequate as sole source.
Testing and Monitoring
Who Should Be Tested
Routine screening of asymptomatic individuals remains controversial and is not universally recommended. Consider testing in:
- Individuals with bone disorders (osteoporosis, osteomalacia, rickets)
- Chronic kidney disease
- Malabsorption syndromes
- Obesity (BMI >30)
- Older adults with history of falls or fractures
- Individuals on medications affecting vitamin D metabolism
- Chronic granulomatous disorders (sarcoidosis, tuberculosis)
- Some lymphomas
- Pregnant women (per some guidelines)
- Individuals with unexplained hypercalcemia or hypercalciuria
Testing Frequency
Initial assessment: Single baseline test before starting supplementation (optional but helpful for determining appropriate dose).
Follow-up after starting supplementation: Retest at 3-4 months to assess response and adjust dose if needed.
Ongoing monitoring:
- If levels are stable and optimal: Annual testing (or less frequent)
- If levels were very low or required high doses: Every 3-6 months until stable
- If on very high doses (>10,000 IU daily): Monitor 25(OH)D and calcium every 3 months
Additional tests to consider:
- Serum calcium
- Parathyroid hormone (PTH)
- 24-hour urinary calcium (if hypercalciuria suspected)
- Kidney function (creatinine, eGFR)
Interpreting Results in Context
A single 25(OH)D measurement represents a snapshot affected by:
- Recent sun exposure
- Supplement adherence
- Seasonal variation
- Assay variability (10-15% between laboratories)
Consider trends over time rather than focusing on single values. The goal is achieving and maintaining levels in the target range, not chasing a specific number.
Special Considerations and Populations
Athletes and Physical Performance
Athletes have higher fracture and stress fracture risk when vitamin D deficient. Some research suggests vitamin D may influence:
- Muscle protein synthesis
- Muscle function and strength
- Injury risk
- Immune function during heavy training
- Inflammatory recovery
A 2019 meta-analysis found vitamin D supplementation improved muscle strength in athletes with baseline deficiency (<30 ng/mL), but not in those already sufficient.33Farrokhyar F, Tabasinejad R, Dao D, et al. Prevalence of vitamin D inadequacy in athletes: a systematic-review and meta-analysis. Sports Med. 2015;45(3):365-378.
Many sports organizations recommend maintaining 25(OH)D levels of 40-50 ng/mL in athletes. For information on supplement testing standards in sports, see our articles on Informed Choice and BSCG Supplement Certification.
Older Adults
Aging affects vitamin D status through:
- Reduced skin synthesis capacity
- Decreased kidney 1α-hydroxylase activity
- Less time outdoors
- Reduced dietary intake
- Impaired intestinal absorption
Falls and fracture prevention become particularly relevant in this population. Combined vitamin D (800-1000 IU daily) plus calcium supplementation shows clearer benefits for fracture reduction in institutionalized elderly than in community-dwelling older adults.
Pregnancy and Lactation
Maternal vitamin D deficiency during pregnancy has been associated with:
- Preeclampsia
- Gestational diabetes
- Preterm birth
- Low birth weight
- Childhood rickets
However, high-quality randomized trials have not definitively established optimal vitamin D levels or supplementation doses during pregnancy. Common recommendations range from 600-2000 IU daily.
Breast milk contains low vitamin D (typically <80 IU/L), insufficient to meet infant needs regardless of maternal status. The American Academy of Pediatrics recommends all breastfed infants receive 400 IU daily vitamin D supplementation starting soon after birth.
Individuals with Darker Skin
Melanin reduces UVB penetration and vitamin D synthesis. African American, Hispanic, and Asian populations living at northern latitudes have substantially higher deficiency rates than Caucasians in the same locations.
A study of African American adults found that 1000 IU daily was insufficient to achieve 25(OH)D levels >20 ng/mL in many participants, while 2000-4000 IU was more effective.34Aloia J, Dhaliwal R, Mikhail M, et al. Free 25(OH)D and the vitamin D paradox in African Americans. J Clin Endocrinol Metab. 2015;100(9):3356-3363.
Interestingly, despite lower 25(OH)D levels, African Americans have higher bone density and lower fracture rates than Caucasians, suggesting possible genetic differences in vitamin D metabolism or calcium regulation. This “vitamin D paradox” complicates interpretation of optimal levels across ethnic groups.
Chronic Kidney Disease
Kidney disease impairs 1α-hydroxylase activity, reducing conversion of 25(OH)D to active calcitriol. Patients with advanced CKD (stages 3-5) often develop:
- Vitamin D deficiency
- Secondary hyperparathyroidism
- Mineral bone disorder
- Vascular calcification
Management requires:
- Maintaining adequate 25(OH)D stores (>30 ng/mL)
- Often requires active vitamin D analogs (calcitriol, paricalcitol) rather than nutritional vitamin D alone
- Careful monitoring of calcium, phosphate, and PTH
- Coordination with nephrologist
Standard vitamin D supplementation is reasonable for CKD stages 1-3, but stages 4-5 require specialist management.
Malabsorption Disorders
Conditions affecting fat absorption impair vitamin D absorption:
Celiac disease: Villous atrophy reduces absorption. Deficiency is common even after gluten-free diet is established. May require 3000-6000 IU daily.
Crohn’s disease: Inflammation and reduced absorptive surface area, especially with ileal involvement. Monitoring and higher doses often needed.
Cystic fibrosis: Pancreatic insufficiency reduces bile acid and lipase availability. Very high doses (up to 10,000-50,000 IU daily) may be required.
Post-bariatric surgery: Particularly after gastric bypass or biliopancreatic diversion. Malabsorption can be severe and lifelong. Doses of 3000-6000 IU daily common, with some patients requiring much more.
These populations benefit from 25(OH)D monitoring every 3-6 months and dose adjustment based on levels.
Controversies and Debates
Optimal Blood Levels
The question of optimal 25(OH)D levels remains contentious:
Conservative position (IOM): ≥20 ng/mL is adequate for bone health in the general population. Higher levels lack proven benefits and may carry unknown risks.
Liberal position (Endocrine Society, some researchers): 30-50 ng/mL is optimal for multiple health outcomes beyond bone, including immune function, cancer prevention, and cardiovascular health.
Evidence gaps: Most research is observational. Randomized trials generally enrolled people with adequate baseline vitamin D, potentially obscuring benefits in deficient individuals. The field lacks large, long-term trials comparing different target levels.
Vitamin D and Mortality
Some observational studies show a U-shaped curve, with both low (<20 ng/mL) and high (>50 ng/mL) 25(OH)D associated with increased mortality. However, this could reflect reverse causality (sicker people have lower vitamin D) or confounding.
Randomized trials have not shown mortality benefits from supplementation in generally healthy populations. A 2019 meta-analysis of 52 trials found no effect of vitamin D on all-cause mortality.35Zhang Y, Fang F, Tang J, et al. Association between vitamin D supplementation and mortality: systematic review and meta-analysis. BMJ. 2019;366:l4673.
Universal Supplementation vs. Targeted Approach
Arguments for universal supplementation:
- High prevalence of deficiency/insufficiency
- Difficulty achieving adequate status through diet and sun alone
- Low cost and safety of 1000-2000 IU daily
- Potential benefits beyond bone health
Arguments against:
- Lack of proven benefits in randomized trials for non-skeletal outcomes
- Most trials show no benefit in those already sufficient
- Risk of creating unnecessary medicalization
- Potential for excessive intake if multiple fortified foods and supplements are combined
Current evidence supports targeted supplementation for:
- Infants (breastfed)
- Elderly with limited sun exposure
- Individuals with documented deficiency
- High-risk groups (dark skin, malabsorption, certain medications)
Whether healthy young adults with adequate sun exposure benefit from routine supplementation remains unclear.
Bolus Dosing Concerns
Studies using large infrequent doses (monthly or yearly) have produced concerning results:
- Increased fall risk in elderly given 500,000 IU annually
- No benefit for fractures or respiratory infections with monthly dosing vs. placebo
- Possible immunosuppressive effects from sudden high calcitriol spikes
These findings suggest that physiological daily dosing is superior to pharmacological boluses, even when the cumulative monthly/yearly dose is equivalent. The human body appears to handle steady intake better than intermittent large doses.
Future Directions and Research
Several areas remain under investigation:
Personalized vitamin D recommendations: Genetic polymorphisms affect vitamin D metabolism (VDR, CYP27B1, CYP24A1, GC genes). Future approaches may tailor supplementation based on individual genetic profiles.
Bioavailable vs. total 25(OH)D: Most 25(OH)D is protein-bound. Some researchers propose that “free” or bioavailable 25(OH)D better predicts health outcomes than total 25(OH)D, potentially explaining ethnic differences in vitamin D requirements.
Vitamin D analogues: Synthetic compounds that activate VDR without causing hypercalcemia are being developed for cancer, autoimmune diseases, and other conditions.
Combination strategies: Research is examining vitamin D combined with other nutrients (K2, magnesium, omega-3s) for synergistic benefits.
Disease-specific trials: Ongoing trials are testing vitamin D in specific populations (critically ill patients, cancer survivors, people with specific autoimmune diseases) where benefits may be clearer than in general population trials.
Conclusion
Vitamin D is essential for calcium homeostasis and bone health, with emerging evidence for broader roles in immune function, cardiovascular health, and chronic disease prevention. The vitamin’s unique dual nature—obtained through both diet and endogenous synthesis—complicates efforts to establish universal recommendations.
Deficiency is common, particularly in older adults, individuals with darker skin, those living at northern latitudes, and people with limited sun exposure or malabsorption disorders. Supplementation clearly benefits those with documented deficiency, especially for bone health and fracture prevention. Evidence for benefits in people who are already sufficient is weaker and more controversial.
Vitamin D3 at doses of 1000-2000 IU daily is safe for most adults and sufficient to maintain adequate status (≥20 ng/mL) in individuals without significant risk factors. Higher doses (2000-4000 IU daily) may be appropriate for those with obesity, malabsorption, limited sun exposure, or other risk factors. Doses above 4000 IU daily should generally be reserved for documented deficiency or used under medical supervision with monitoring.
Testing can identify individuals who need supplementation and guide appropriate dosing, though universal screening remains debated. For those who supplement, vitamin D3 is preferred over D2, daily dosing is superior to large bolus doses, and taking supplements with dietary fat enhances absorption.
The balance between ensuring adequate vitamin D status and avoiding excessive supplementation requires individual assessment of risk factors, dietary intake, sun exposure patterns, and when appropriate, blood testing.
For personalized supplement recommendations based on your individual health profile and goals, consider using our Smart Stack Builder tool.
Frequently Asked Questions
What’s the difference between vitamin D2 and D3?
Vitamin D2 (ergocalciferol) comes from plant sources, while D3 (cholecalciferol) is synthesized in animal skin or found in animal-based foods. Research shows D3 is approximately 87% more effective at raising and maintaining blood levels of vitamin D. For supplementation, D3 is generally preferred unless you follow a strict vegan diet.
Can I get enough vitamin D from the sun?
It depends on your location, skin tone, age, and lifestyle. During summer months at lower latitudes, 10-30 minutes of midday sun exposure on 25% of your body several times weekly can produce adequate vitamin D for light-skinned individuals. However, geographic location (especially above 37°N), winter months, darker skin, sunscreen use, indoor lifestyle, and aging all reduce skin production. Most dermatologists recommend supplementation over unprotected sun exposure due to skin cancer risks.
How long does it take to correct vitamin D deficiency?
With daily supplementation of 2000-4000 IU, levels typically increase within days, but reaching optimal status takes 2-3 months. Severe deficiency (<10 ng/mL) may be treated with 50,000 IU weekly for 8-12 weeks, followed by maintenance dosing. Testing at 3 months after starting supplementation shows whether the dose is adequate.
Should I take vitamin D with food?
Yes. Vitamin D is fat-soluble and absorption increases by 32-56% when taken with a meal containing fat. Even a small amount of fat (11g, about one tablespoon of olive oil or a handful of nuts) is sufficient. Taking vitamin D on an empty stomach reduces how much your body absorbs.
Can I take too much vitamin D?
Yes, though toxicity is rare. Doses up to 4000 IU daily are considered safe for long-term use in adults. Toxicity typically requires chronic intake exceeding 10,000-40,000 IU daily for months, causing hypercalcemia (elevated blood calcium). Symptoms include nausea, vomiting, weakness, and kidney problems. You cannot get vitamin D toxicity from sun exposure—only from excessive supplementation.
What vitamin D level should I aim for?
This is debated. The Institute of Medicine considers ≥20 ng/mL adequate for bone health. The Endocrine Society recommends 30-50 ng/mL for optimal health. Most experts agree that levels below 20 ng/mL indicate deficiency requiring treatment, and levels above 100 ng/mL carry toxicity risk. A target of 30-50 ng/mL balances potential benefits against uncertainty about very high levels.
Do I need to take vitamin K2 with vitamin D?
This is an area of active research. Vitamin K2 activates proteins that direct calcium into bones and away from soft tissues, which theoretically complements vitamin D’s role in calcium absorption. Some researchers recommend combining them, especially at higher vitamin D doses (>2000 IU daily), but definitive evidence is lacking. It’s not strictly necessary but may be beneficial.
Why is my vitamin D still low despite supplementation?
Several factors can reduce response to supplementation: taking it without fat (poor absorption), malabsorption disorders (celiac disease, Crohn’s disease, cystic fibrosis, gastric bypass), obesity (vitamin D sequestered in fat tissue), certain medications (anticonvulsants, corticosteroids), or magnesium deficiency (impairs vitamin D activation). Very rarely, genetic variants affect vitamin D metabolism. Testing after 3 months of supplementation can identify non-responders who need higher doses or further evaluation.
Is vitamin D dangerous for people with kidney stones?
Vitamin D increases calcium absorption, which could theoretically increase kidney stone risk in susceptible individuals. However, research shows that normal supplementation doses (1000-2000 IU daily) do not increase stone risk in most people. Those with a history of calcium-based kidney stones should maintain adequate hydration, avoid excessive calcium supplementation, and may benefit from monitoring urinary calcium excretion if taking high-dose vitamin D.
Can vitamin D help with depression or mood?
Some studies show that vitamin D supplementation reduces depression symptoms, particularly in people with clinical depression and baseline deficiency. A 2020 meta-analysis found small-to-moderate benefits. Effects are most apparent in those with 25(OH)D <20 ng/mL taking doses ≥2000 IU daily. Vitamin D is not a replacement for standard depression treatment but may be a useful adjunct, especially if you’re deficient.
Should pregnant women take vitamin D?
Vitamin D deficiency during pregnancy has been associated with preeclampsia, gestational diabetes, and other complications. Most prenatal vitamins contain 400-600 IU, but many experts recommend 1000-2000 IU daily for pregnant women. The American College of Obstetricians and Gynecologists states that 1000-2000 IU daily is safe. Discuss supplementation with your obstetrician, particularly if you have risk factors for deficiency.
Does vitamin D interact with medications?
Yes. Several medications reduce vitamin D levels (corticosteroids, anticonvulsants like phenytoin, some HIV drugs, orlistat) or are affected by vitamin D (thiazide diuretics, digoxin). Vitamin D can also interact with hydroxychloroquine. If you take any medications chronically, discuss vitamin D supplementation with your healthcare provider and consider monitoring calcium levels.
Can children take vitamin D supplements?
Yes. The American Academy of Pediatrics recommends 400 IU daily for all infants starting shortly after birth, continuing through childhood and adolescence. Breastfed infants particularly need supplementation since breast milk contains minimal vitamin D. Children with obesity, dark skin, limited sun exposure, or certain medical conditions may need higher doses. Always use age-appropriate formulations and dosing.
How should I store vitamin D supplements?
Store vitamin D in a cool, dry place away from direct light and heat. Bathroom medicine cabinets (often warm and humid) are not ideal. Oil-based softgels are generally more stable than dry tablets. Most supplements maintain potency for 2-3 years when stored properly. Check expiration dates and discard outdated supplements.
If I have high vitamin D, should I stop supplementing immediately?
If your level is moderately elevated (50-80 ng/mL), simply reduce or stop supplementation and retest in 2-3 months. Levels will decline gradually (half-life of 2-3 weeks). If your level is very high (>100 ng/mL) or you have symptoms of toxicity, stop supplementation and contact your healthcare provider. They may check your calcium levels and kidney function. Very high levels without supplementation could indicate other medical conditions requiring evaluation.
References
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34Aloia J, Dhaliwal R, Mikhail M, et al. Free 25(OH)D and the vitamin D paradox in African Americans. J Clin Endocrinol Metab. 2015;100(9):3356-3363.
- 35Zhang Y, Fang F, Tang J, et al. Association between vitamin D supplementation and mortality: systematic review and meta-analysis. BMJ. 2019;366:l4673.
Apply This Research to Your Stack
Use Smart Stack Builder to create a personalized supplement schedule based on your specific goals. Get timing recommendations, interaction warnings, and dosage guidance: all grounded in the research you just read.
This article is part of our Supplements hub — A science-backed collection of ingredient research, clinical dosage reviews, and optimized stack insights..
Questions or Comments?
If you have a question or comment about this article, feel free to leave it below. All comments are moderated for clarity, accuracy, and relevance.