Biotin Supplementation: The Complete Scientific Guide to Evidence and What the Research Actually Shows
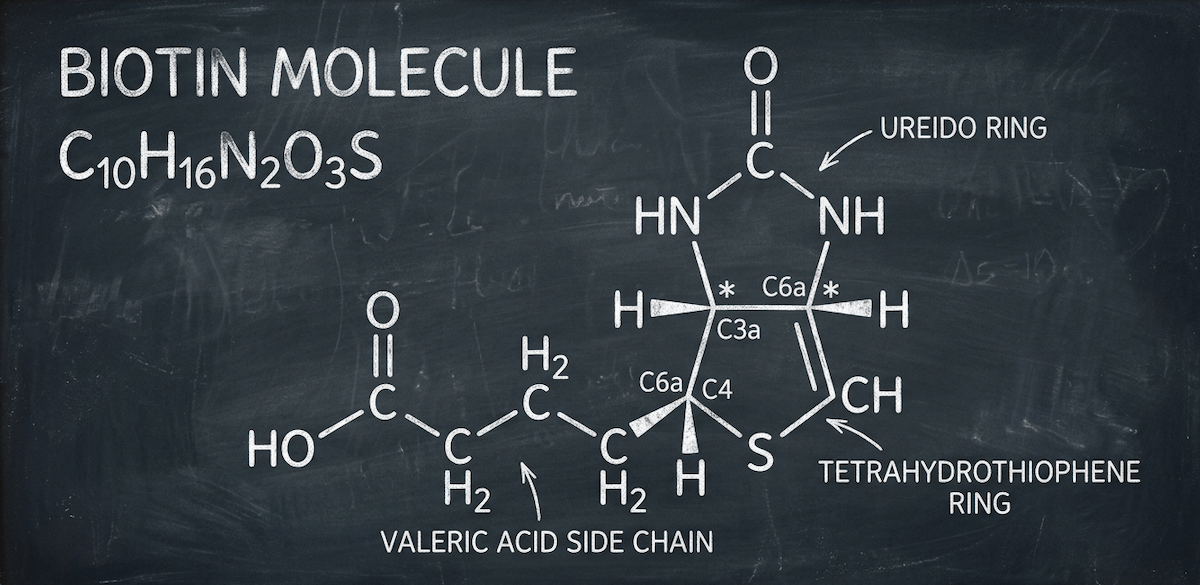
Biotin sits at the center of one of the most striking disconnects in modern supplement science: a nearly $2 billion global market built almost entirely on consumer demand for hair, skin, and nail benefits, with virtually no randomized controlled trial evidence supporting those claims in healthy individuals. Known variously as vitamin B7, vitamin H (from the German Haar und Haut, meaning “hair and skin”), and coenzyme R, biotin is a water-soluble B vitamin that serves as an essential cofactor for carboxylase enzymes involved in critical metabolic pathways including gluconeogenesis, fatty acid synthesis, and amino acid catabolism1Zempleni, J., et al. “Biotin and biotinidase deficiency.” Expert Review of Endocrinology & Metabolism, 2008; 3(6): 715-724..
The scientific reality of biotin supplementation is far more nuanced, and far more interesting, than the marketing suggests. While biotin is unquestionably essential for human health, and genuine deficiency produces dramatic symptoms including hair loss, dermatitis, and neurological dysfunction, the leap from “necessary nutrient” to “take 10,000 mcg daily for longer hair” rests on remarkably thin evidence. Meanwhile, emerging research into biotin’s roles in glucose metabolism, gene regulation, and immune function suggests the vitamin’s most promising therapeutic applications may have nothing to do with cosmetic outcomes at all.
This analysis examines the full landscape of biotin research: the legitimate biochemistry, the evidence gaps, the genuine safety concerns that most supplement marketers ignore, and the emerging therapeutic applications that deserve more attention than they currently receive. Our goal, as always, is to give you the data you need to make informed decisions rather than profitable ones.
Biochemistry and Metabolic Roles
Biotin as a Carboxylase Cofactor
Biotin’s fundamental biochemical role involves serving as a covalently bound prosthetic group for four carboxylase enzymes in humans, each catalyzing a critical carbon dioxide transfer reaction in intermediary metabolism. A fifth enzyme, holocarboxylase synthetase, is responsible for attaching biotin to these carboxylases. Together, this system represents biotin’s established, uncontroversial mechanism of action, the foundation upon which all other claims must be evaluated2Tong, L. “Structure and function of biotin-dependent carboxylases.” Cellular and Molecular Life Sciences, 2013; 70(5): 863-891..
The five biotin-dependent carboxylases and their metabolic roles are as follows:
Acetyl-CoA Carboxylase (ACC) catalyzes the first committed step of fatty acid synthesis, converting acetyl-CoA to malonyl-CoA. Two isoforms exist: ACC1 (cytosolic, primary fatty acid synthesis) and ACC2 (mitochondrial outer membrane, regulation of fatty acid oxidation). This enzyme’s dependence on biotin provides the mechanistic rationale for biotin’s proposed roles in lipid metabolism and, by extension, myelin synthesis, the basis for the multiple sclerosis research discussed later3Wakil, S.J., & Abu-Elheiga, L.A. “Fatty acid metabolism: target for metabolic syndrome.” Journal of Lipid Research, 2009; 50 Suppl: S138-S143..
Pyruvate Carboxylase (PC) converts pyruvate to oxaloacetate, replenishing the citric acid cycle and serving as the first step of gluconeogenesis. This enzyme is critical for maintaining blood glucose levels during fasting and is the primary link between biotin status and glucose metabolism, an area of genuine therapeutic interest4Jitrapakdee, S., et al. “Structure, mechanism and regulation of pyruvate carboxylase.” Biochemical Journal, 2008; 413(3): 369-387..
Propionyl-CoA Carboxylase (PCC) converts propionyl-CoA to methylmalonyl-CoA in the catabolism of odd-chain fatty acids, certain amino acids (isoleucine, valine, methionine, threonine), and cholesterol side chains. Deficiency of this enzyme causes propionic acidemia, a serious inherited metabolic disorder5Desviat, L.R., et al. “Propionic acidemia: mutation update and functional and structural effects of the variant alleles.” Molecular Genetics and Metabolism, 2004; 83(1-2): 28-37..
3-Methylcrotonyl-CoA Carboxylase (MCC) functions in the catabolism of leucine, converting 3-methylcrotonyl-CoA to 3-methylglutaconyl-CoA. This enzyme’s biotin dependence links the vitamin to branched-chain amino acid metabolism6Baumgartner, M.R., et al. “The molecular basis of human 3-methylcrotonyl-CoA carboxylase deficiency.” Journal of Clinical Investigation, 2001; 107(4): 495-504..
Holocarboxylase Synthetase (HCS) is technically not a carboxylase itself but rather the enzyme responsible for covalently attaching biotin to all five carboxylases. Deficiency of HCS produces multiple carboxylase deficiency, a condition that mimics severe biotin deficiency and responds dramatically to high-dose biotin supplementation7Suzuki, Y., et al. “Mutations in the holocarboxylase synthetase gene HLCS.” Human Mutation, 2005; 26(4): 285-290..
Beyond Carboxylase Function: Epigenetic and Gene Regulatory Roles
Research over the past two decades has revealed that biotin’s biological functions extend well beyond its classical role as a carboxylase cofactor. Biotin participates in histone modification, gene regulation, and cell signaling, functions that, while scientifically fascinating, are frequently overstated in supplement marketing8Zempleni, J., et al. “Biotin.” BioFactors, 2009; 35(1): 36-46..
Histone Biotinylation: Biotinidase and holocarboxylase synthetase can attach biotin to specific lysine residues on histones H2A, H3, and H4. This epigenetic modification appears to play roles in gene silencing, DNA repair, and chromatin stability. However, the extent to which dietary biotin status influences histone biotinylation in humans, and whether supplementation beyond adequacy provides any additional epigenetic benefit, remains unclear9Camporeale, G., et al. “K12-biotinylated histone H4 marks heterochromatin in human lymphoblastoma cells.” Journal of Nutritional Biochemistry, 2007; 18(11): 760-768..
Gene Expression Regulation: Biotin status affects the expression of over 2,000 genes in human cells, including genes involved in biotin transport, cell signaling, chromatin structure, and immune function. At pharmacological concentrations, biotin can modulate the expression of glucokinase in hepatocytes and pancreatic beta cells, an effect with legitimate implications for glucose metabolism that has nothing to do with hair growth10Romero-Navarro, G., et al. “Biotin regulation of pancreatic glucokinase and insulin in primary cultured rat islets and in biotin-deficient rats.” Endocrinology, 1999; 140(10): 4595-4600..
Cell Signaling: Biotin influences several cell signaling pathways, including NF-κB, which plays central roles in inflammation and immune function. Biotin deficiency has been shown to increase NF-κB activity and pro-inflammatory cytokine production, while supplementation may attenuate these effects. These observations have prompted research into biotin’s potential immunomodulatory properties, though clinical translation remains limited11Rodriguez-Melendez, R., & Zempleni, J. “Regulation of gene expression by biotin.” Journal of Nutritional Biochemistry, 2003; 14(12): 680-690..
Absorption, Transport, and Metabolism
Dietary biotin exists in both free and protein-bound forms. Protein-bound biotin is released by proteolytic digestion and the action of biotinidase in the intestinal lumen, yielding free biotin for absorption12Said, H.M. “Biotin: biochemical, physiological and clinical aspects.” Subcellular Biochemistry, 2011; 56: 1-19..
Free biotin is absorbed in the small intestine via the sodium-dependent multivitamin transporter (SMVT), encoded by the SLC5A6 gene. This transporter also handles pantothenic acid (vitamin B5) and lipoic acid, creating potential competitive interactions at very high supplemental doses. Absorption is highly efficient at physiological concentrations but becomes proportionally less efficient at the megadoses common in supplements, meaning that much of a 10,000 mcg supplement is excreted unabsorbed13Prasad, P.D., et al. “Cloning and functional expression of a cDNA encoding a mammalian sodium-dependent vitamin transporter mediating the uptake of pantothenate, biotin, and lipoate.” Journal of Biological Chemistry, 1998; 273(13): 7501-7506..
The intestinal microbiome also synthesizes biotin, though the contribution of bacterially produced biotin to human requirements remains debated. Some evidence suggests that bacterial biotin synthesis in the large intestine can be absorbed via a colonic SMVT, potentially contributing to biotin status, which may partly explain why frank biotin deficiency is relatively rare even in individuals with marginal dietary intake14Said, H.M., & Mohammed, Z.M. “Intestinal absorption of water-soluble vitamins: an update.” Current Opinion in Gastroenterology, 2006; 22(2): 140-146..
As a water-soluble vitamin, biotin is not stored in significant quantities in the body. Excess biotin is excreted primarily in urine, both as free biotin and as the metabolites bisnorbiotin and biotin sulfoxide. This rapid excretion is the basis for the generally accepted view that biotin has low toxicity, though as we will discuss, “low toxicity” is not the same as “no risk.”
Dietary Sources and Requirements
Adequate Intake and Dietary Sources
Biotin lacks a Recommended Dietary Allowance (RDA) because insufficient data exist to establish an Estimated Average Requirement. Instead, the Institute of Medicine set an Adequate Intake (AI) of 30 mcg/day for adults, a value based on estimated dietary intakes in healthy populations rather than dose-response studies of functional outcomes15Institute of Medicine. “Dietary Reference Intakes for Thiamin, Riboflavin, Niacin, Vitamin B6, Folate, Vitamin B12, Pantothenic Acid, Biotin, and Choline.” National Academies Press, 1998..
This is an important distinction. The 30 mcg AI does not represent a carefully determined threshold below which deficiency symptoms appear. It is simply an estimate of what most healthy people seem to consume. This uncertainty about true requirements is one reason why supplement marketers can claim that higher intakes might provide benefits, there is genuinely insufficient data to prove them wrong, even if there is equally insufficient data to prove them right.
Biotin is widely distributed in foods, though at relatively low concentrations. A typical Western diet provides approximately 35-70 mcg of biotin daily, well above the AI16Staggs, C.G., et al. “Determination of the biotin content of select foods using accurate and sensitive HPLC/avidin binding.” Journal of Food Composition and Analysis, 2004; 17(6): 767-776.. Particularly rich dietary sources include egg yolks (approximately 13-25 mcg per yolk), liver and organ meats (30-100 mcg per serving), nuts and seeds (particularly almonds and peanuts), legumes (especially soybeans), whole grains, and some vegetables including sweet potatoes and spinach.
A notable quirk of biotin nutrition involves raw egg whites, which contain avidin, a glycoprotein that binds biotin with extraordinary affinity (Kd ≈ 10⁻¹⁵ M), effectively rendering it unavailable for absorption. Cooking denatures avidin, eliminating this interaction. The theoretical concern about egg white consumption and biotin deficiency requires consumption of approximately 12 or more raw egg whites daily for extended periods, a scenario that is, to put it mildly, unusual outside of certain bodybuilding subcultures and early 20th-century nutritional experiments17Eakin, R.E., et al. “Egg-white injury in chicks and its relationship to a deficiency of vitamin H (biotin).” Science, 1940; 92(2394): 224-225..
Biotin Deficiency: Rare but Real
Frank biotin deficiency is uncommon in industrialized countries but does occur in specific clinical scenarios. Understanding who actually develops deficiency is essential for evaluating supplementation claims, because the dramatic responses to biotin in deficient individuals are routinely extrapolated to justify supplementation in non-deficient populations, a logical error that pervades biotin marketing18Mock, D.M. “Biotin: From Nutrition to Therapeutics.” Journal of Nutrition, 2017; 147(8): 1487-1492..
Established Risk Factors for Deficiency:
Inherited enzyme deficiencies represent the most severe form of biotin-related pathology. Biotinidase deficiency (estimated incidence 1:60,000) and holocarboxylase synthetase deficiency impair either biotin recycling or attachment to carboxylases, respectively. Both conditions cause multiple carboxylase deficiency with symptoms including seizures, hypotonia, developmental delay, alopecia, and dermatitis. These conditions respond dramatically to high-dose biotin supplementation (10,000-30,000 mcg/day), and their management represents biotin’s most unambiguous therapeutic success19Wolf, B. “Biotinidase deficiency: ‘If you have to have an inherited metabolic disease, this is the one to have.'” Genetics in Medicine, 2012; 14(6): 565-575..
Pregnancy represents a relatively common scenario of marginal biotin depletion. Studies using sensitive biomarkers (3-hydroxyisovaleric acid excretion, decreased lymphocyte propionyl-CoA carboxylase activity) suggest that a substantial proportion of pregnant women develop marginal biotin deficiency despite normal dietary intake. The clinical significance of this marginal depletion, and whether supplementation beyond prenatal vitamin amounts provides benefit, remains under investigation20Mock, D.M. “Marginal biotin deficiency is common in normal human pregnancy and is highly teratogenic in mice.” Journal of Nutrition, 2009; 139(1): 154-157..
Prolonged parenteral nutrition without biotin supplementation historically caused deficiency, though modern parenteral formulations include biotin. Prolonged anticonvulsant therapy (particularly valproic acid, carbamazepine, and phenytoin) can impair biotin status through increased catabolism and decreased absorption. Chronic alcoholism impairs biotin absorption and increases urinary excretion. Inflammatory bowel disease and other conditions affecting intestinal absorption can reduce biotin uptake21Mock, D.M., et al. “Biotin deficiency: an unusual complication of parenteral alimentation.” New England Journal of Medicine, 1981; 304(14): 820-823..
Isotretinoin therapy deserves special mention because it creates a scenario where biotin supplementation for hair-related concerns may have some rational basis. Studies have demonstrated that isotretinoin significantly reduces biotinidase activity, and isotretinoin-associated telogen effluvium may be partially mediated by this mechanism22Schulpis, K.H., et al. “The effect of isotretinoin on biotinidase activity.” Skin Pharmacology and Applied Skin Physiology, 1999; 12(1-2): 28-33..
Symptoms of Deficiency: When genuine deficiency occurs, the clinical presentation is distinctive and includes perioral dermatitis (a scaly, erythematous rash around the mouth, nose, and eyes), alopecia (often progressive and diffuse), conjunctivitis, neurological symptoms (depression, lethargy, hallucinations, paresthesias), and in severe cases, immune dysfunction with increased susceptibility to infections. These symptoms resolve with biotin replacement, a clinical observation that, while dramatic, does not support supplementation in individuals without deficiency.
Hair, Skin, and Nails: The Evidence Gap
The Marketing Narrative vs. The Research Reality
The global biotin supplement market is projected to exceed $4 billion by 2034, driven almost entirely by consumer demand for hair, skin, and nail benefits. Social media promotion, influencer endorsements, and the “beauty-from-within” marketing trend have created enormous consumer awareness, and expectation, around biotin’s cosmetic effects. The question is whether the science supports the spending23Soleymani, T., et al. “The Infatuation With Biotin Supplementation: Is There Truth Behind Its Rising Popularity? A Comparative Analysis of Clinical Efficacy versus Social Popularity.” Journal of Drugs in Dermatology, 2017; 16(5): 496-500..
The answer, based on current evidence, is straightforward: no randomized controlled trial has demonstrated that biotin supplementation improves hair growth or quality in healthy individuals without biotin deficiency. This is not a subtle finding buried in statistical nuances. It is the complete absence of the evidence that would be needed to support the claims being made.
A systematic review published in the Journal of Clinical and Aesthetic Dermatology examined all published studies specifically investigating oral biotin for hair growth or quality. After excluding case reports and case series, only three studies met inclusion criteria. The highest-quality study, a double-blind, placebo-controlled trial, found no difference between biotin and placebo groups for hair growth. The other two studies investigated specific patient populations (isotretinoin users and post-bariatric surgery patients) and were susceptible to multiple potential biases24Yelich, A., et al. “Biotin for Hair Loss: Teasing Out the Evidence.” Journal of Clinical and Aesthetic Dermatology, 2024; 17(8): 56-61..
An earlier systematic review identified 18 reported cases of biotin supplementation for hair and nail changes. In every single case, the patient had an underlying pathology for poor hair or nail growth, biotinidase deficiency, holocarboxylase synthetase deficiency, uncombable hair syndrome, or acquired biotin deficiency from specific causes. While all cases showed clinical improvement after receiving biotin, none represented supplementation in otherwise healthy individuals25Patel, D.P., et al. “A Review of the Use of Biotin for Hair Loss.” Skin Appendage Disorders, 2017; 3(3): 166-169..
Why the Evidence Gap Persists
Several factors explain why biotin’s cosmetic claims remain unsupported despite the supplement’s massive market presence.
No financial incentive for rigorous trials: Biotin is a generic compound that cannot be patented. Supplement companies profit from consumer demand without needing to fund expensive clinical trials, the regulatory framework for dietary supplements does not require efficacy data before marketing. The absence of evidence is not evidence of absence, but it is also not a substitute for evidence of efficacy.
Confounding by deficiency correction: The most dramatic responses to biotin supplementation occur in individuals with genuine deficiency or borderline status. In any uncontrolled study or anecdotal report, the subset of participants who happen to be marginally deficient may show genuine improvement, creating the impression of a general benefit that does not extend to the biotin-replete majority.
Placebo effects and expectation bias: Hair growth is a slow process (approximately 1 cm per month), and subjective assessment of hair quality is highly susceptible to expectation bias. When someone begins taking a supplement they believe will improve their hair, they tend to observe improvements, whether or not they are occurring. Only blinded, placebo-controlled trials with objective outcome measures can distinguish real effects from perceived ones.
Confounding by multi-ingredient products: Many studies reporting positive results used combination products containing biotin alongside zinc, iron, marine proteins, saw palmetto, or other ingredients with independent evidence for hair health effects. Attributing observed benefits to biotin specifically in these contexts is impossible without appropriate factorial designs26Ablon, G. “A 3-Month, Randomized, Double-Blind, Placebo-Controlled Study Evaluating the Ability of an Extra-Strength Marine Protein Supplement to Promote Hair Growth and Decrease Shedding in Women with Self-Perceived Thinning Hair.” Dermatology Research and Practice, 2015; 2015: 841570..
Nail Health: Slightly Better Evidence, Still Limited
The evidence for biotin’s effects on nail health is marginally stronger than for hair, though it remains limited to a small number of studies in individuals with brittle nails.
The most frequently cited study, by Colombo et al. (1990), examined 44 patients with brittle nails treated with 2,500 mcg of biotin daily. After an average of 5.5 months of treatment, nail thickness increased by 25% as measured by electron microscopy, and 91% of participants reported improvement. However, this study lacked a control group, making it impossible to distinguish biotin’s effects from natural variation, placebo effects, or other concurrent changes27Colombo, V.E., et al. “Treatment of brittle fingernails and onychoschizia with biotin: scanning electron microscopy.” Journal of the American Academy of Dermatology, 1990; 23(6 Pt 1): 1127-1132..
A subsequent study by Hochman et al. (1993) found that biotin supplementation (2,500 mcg/day) increased nail plate thickness by approximately 25% in patients with brittle nails after 6-15 months of treatment. Again, the study lacked placebo control28Hochman, L.G., et al. “Brittle nails: response to daily biotin supplementation.” Cutis, 1993; 51(4): 303-305..
While these results suggest a possible benefit for brittle nails specifically, the absence of placebo-controlled data prevents definitive conclusions. The evidence is best described as suggestive but unconfirmed, and it applies specifically to individuals with diagnosed brittle nail syndrome, not to the general population seeking cosmetic improvement.
The Safety Concern Nobody Talks About: Lab Test Interference
A Clinically Significant and Under-Recognized Risk
While biotin’s low acute toxicity is well-established, it is a water-soluble vitamin that is rapidly excreted, the most clinically significant risk of biotin supplementation has nothing to do with the vitamin’s direct biological effects. High-dose biotin causes interference with a wide range of commonly used clinical laboratory tests, producing results that can be profoundly and dangerously misleading. This is not a theoretical concern: at least one death has been reported to the FDA as potentially related to biotin-induced laboratory interference29U.S. Food and Drug Administration. “UPDATE: The FDA Warns that Biotin May Interfere with Lab Tests: FDA Safety Communication.” November 2019..
The mechanism is straightforward. Many modern immunoassays use the streptavidin-biotin interaction as a capture or detection system. When a patient’s blood contains elevated biotin from supplementation, this exogenous biotin competes with the biotin in the assay system, producing inaccurate results. The direction of the error depends on the assay design: competitive immunoassays (used for small molecules like free T4, free T3) produce falsely elevated results, while sandwich immunoassays (used for large molecules like TSH, troponin) produce falsely decreased results30Li, D., et al. “Association of Biotin Ingestion With Performance of Hormone and Nonhormone Assays in Healthy Adults.” JAMA, 2017; 318(12): 1150-1160..
Which Tests Are Affected
The range of laboratory tests susceptible to biotin interference is disturbingly broad and includes some of the most clinically consequential assays in medicine31Samarasinghe, S., et al. “Biotin Interference with Routine Clinical Immunoassays: Understand the Causes and Mitigate the Risks.” Endocrine Practice, 2017; 23(8): 989-998..
Thyroid Function Tests: Biotin interference can produce a pattern of elevated free T4 and free T3 with suppressed TSH, a pattern indistinguishable from hyperthyroidism. Published case reports describe patients who received unnecessary antithyroid treatment, underwent repeated imaging and biopsies, and endured months of diagnostic confusion before biotin interference was identified as the cause. In patients with thyroid cancer being monitored by thyroglobulin levels, biotin interference could mask recurrence or produce false alarms, either of which could have devastating consequences32Barbesino, G. “Misdiagnosis of Graves’ Disease with Apparent Severe Hyperthyroidism in a Patient Taking Biotin Megadoses.” Thyroid, 2016; 26(6): 860-863..
Cardiac Troponin: Perhaps the most dangerous interference involves cardiac troponin assays, which are the primary diagnostic tool for myocardial infarction (heart attack). Biotin can produce falsely low troponin results, potentially causing a clinician to miss an active heart attack. The FDA has specifically highlighted this risk, noting ongoing adverse event reports of biotin causing falsely low troponin results. The agency maintains a public list of troponin assays that remain susceptible to biotin interference33U.S. Food and Drug Administration. “Biotin Interference with Troponin Lab Tests – Assays Subject to Biotin Interference.”.
Other Affected Tests: The list extends to parathyroid hormone, testosterone, estradiol, cortisol, DHEA-S, progesterone, β-hCG (pregnancy tests), ferritin, folate, vitamin B12, PSA, various cancer markers (CA-125, CA 19-9, AFP), hepatitis B and C serologies, and HIV serology. For any patient taking high-dose biotin supplements, essentially any laboratory result generated by an immunoassay platform should be interpreted with caution34AACC (Association for Diagnostics & Laboratory Medicine). “AACC Guidance Document on Biotin Interference in Laboratory Tests.” Journal of Applied Laboratory Medicine, 2020; 5(3): 575-587..
Dose Thresholds and Practical Implications
Biotin doses found in standard multivitamins (typically 30-300 mcg) have not been reported to cause clinically significant assay interference. The risk increases substantially with the high-dose supplements marketed for hair, skin, and nail benefits, which commonly contain 5,000-10,000 mcg (5-10 mg), doses 167 to 333 times the Adequate Intake. Some supplements contain up to 20,000 mcg (20 mg), or more than 650 times the AI35Katzman, B.M., et al. “Prevalence of biotin supplement usage in outpatients and plasma biotin concentrations in patients presenting to the emergency department.” Clinical Biochemistry, 2018; 60: 11-16..
A Mayo Clinic survey found that 7.7% of outpatients used biotin-containing supplements, and analysis of emergency department plasma samples revealed that approximately 7% of patients had biotin concentrations capable of interfering with certain laboratory tests. Critically, surveys indicate that only 6% of patients taking biotin had been informed about potential lab test interference, and 19% of physicians prescribing biotin were unaware of the interaction36Chun, K.Y. “Biotin interference in diagnostic tests.” Clinical Chemistry, 2017; 63(2): 619-620..
Practical guidance for biotin supplement users: If you take biotin supplements at doses above 1,000 mcg, you should disclose this to any healthcare provider ordering laboratory tests, and ideally discontinue biotin for at least 24-72 hours before blood draws. For doses of 10 mg or more, some experts recommend discontinuation for one week before testing. In an emergency setting where lab tests cannot be delayed, informing the laboratory about biotin use is essential. The 2025-2026 FDA Safety Communications update has mandated clearer labeling for high-dose biotin products (above 5,000 mcg) specifically because of this interference risk.
Glucose Metabolism and Diabetes: The Underappreciated Research
Mechanistic Basis for Glycemic Effects
While the cosmetic claims dominate public awareness, some of the most scientifically interesting biotin research involves its effects on glucose metabolism, a domain with genuine mechanistic plausibility and emerging clinical data that, while preliminary, deserves more attention than it receives37Fernandez-Mejia, C. “Pharmacological effects of biotin.” Journal of Nutritional Biochemistry, 2005; 16(7): 424-427..
Biotin influences glucose metabolism through two primary pathways. First, pharmacological doses of biotin upregulate the expression of glucokinase in both hepatocytes and pancreatic beta cells. Glucokinase is the rate-limiting enzyme for glucose phosphorylation in these tissues and is critical for glucose-stimulated insulin secretion, postprandial hepatic glucose uptake, and suppression of hepatic glucose output. Diabetic patients frequently have subnormal hepatic glucokinase activity, and biotin’s ability to enhance glucokinase expression provides a clear mechanistic link between the vitamin and glucose homeostasis38Dakshinamurti, K., & Chauhan, J. “Regulation of biotin enzymes.” Annual Review of Nutrition, 1988; 8: 211-233..
Second, biotin serves as the essential cofactor for pyruvate carboxylase, the gateway enzyme for gluconeogenesis. At pharmacological concentrations, biotin can also repress the expression of gluconeogenic genes (including phosphoenolpyruvate carboxykinase, glucose-6-phosphatase, and their transcription factors FoxO1 and HNF4α) through a pathway that appears to be independent of insulin signaling, a potentially significant finding for individuals with insulin resistance39Sugita, Y., et al. “Effect of biotin treatment on hepatic gene expression in streptozotocin-induced diabetic rats.” Bioscience, Biotechnology, and Biochemistry, 2008; 72(5): 1290-1298..
Additionally, supraphysiological concentrations of biotin can activate soluble guanylate cyclase, increasing cGMP levels and enhancing glucose uptake in muscle cells. This mechanism has been demonstrated in cell culture and animal models but awaits clinical confirmation40Lazo de la Vega-Monroy, M.L., et al. “Effects of biotin supplementation in the diet on insulin secretion, islet gene expression, glucose homeostasis and beta-cell proportion.” Journal of Nutritional Biochemistry, 2013; 24(1): 169-177..
Clinical Evidence in Type 2 Diabetes
Human clinical data on biotin and glucose metabolism, while more limited than the preclinical evidence, shows consistent directional effects that warrant further investigation.
An early clinical study by Maebashi et al. evaluated biotin supplementation (9 mg/day) in 43 patients with non-insulin-dependent diabetes. The investigators found that supplementation significantly reduced fasting blood glucose levels while also decreasing serum pyruvate and lactate concentrations, consistent with enhanced pyruvate carboxylase activity. Notably, serum biotin levels in the diabetic patients were significantly lower than in healthy controls at baseline and inversely correlated with fasting glucose41Maebashi, M., et al. “Therapeutic Evaluation of the Effect of Biotin on Hyperglycemia in Patients with Non-Insulin Dependent Diabetes Mellitus.” Journal of Clinical Biochemistry and Nutrition, 1993; 14(3): 211-218..
A 2022 systematic review and meta-analysis examining biotin’s effects on glycemic control and lipid profiles in type 2 diabetes pooled data from available trials and found consistent trends toward reduced fasting blood glucose and improvements in lipid parameters, though the authors noted significant heterogeneity between studies and called for larger, higher-quality trials42Chen, S., et al. “Influence of biotin intervention on glycemic control and lipid profile in patients with type 2 diabetes mellitus: A systematic review and meta-analysis.” Frontiers in Nutrition, 2022; 9: 1046800..
The combination of chromium picolinate and biotin has received particular attention, with several trials demonstrating improved glycemic control and lipid profiles in type 2 diabetes. One well-designed study found that 30 days of supplementation with 600 mcg chromium picolinate plus 2 mg biotin significantly reduced fasting glucose and coronary risk factors, with additional improvements in HbA1c observed at 90 days43Singer, G.M., & Geohas, J. “The effect of chromium picolinate and biotin supplementation on glycemic control in poorly controlled patients with type 2 diabetes mellitus: a placebo-controlled, double-blinded, randomized trial.” Diabetes Technology & Therapeutics, 2006; 8(6): 636-643..
Critical Caveats: These findings, while promising, require significant qualification. Most studies are small, some lack adequate blinding, and the doses used (2-16 mg/day) are well within the range that causes lab test interference, creating a genuine clinical dilemma for diabetic patients who would need regular laboratory monitoring. Additionally, the interaction between biotin supplementation and diabetes medications (particularly those that lower blood glucose) has not been systematically studied, raising concerns about hypoglycemia risk. Any diabetic patient considering biotin supplementation should do so only under medical supervision.
Multiple Sclerosis: The Rise and Fall of High-Dose Biotin
The MD1003 Story
The investigation of pharmaceutical-grade high-dose biotin (MD1003, 100 mg three times daily = 300 mg/day, or 10,000 times the AI) for progressive multiple sclerosis represents one of the more instructive recent chapters in neuropharmacology, a story of genuine mechanistic plausibility, initial encouraging results, and ultimate failure to confirm efficacy in definitive trials44Sedel, F., et al. “High doses of biotin in chronic progressive multiple sclerosis: a pilot study.” Multiple Sclerosis and Related Disorders, 2015; 4(2): 159-169..
The rationale was sound: biotin activates acetyl-CoA carboxylase, the rate-limiting enzyme in fatty acid synthesis, which is required for myelin production. By enhancing fatty acid synthesis in oligodendrocytes (the cells that produce myelin in the central nervous system), high-dose biotin might promote remyelination, a therapeutic goal that no existing MS treatment adequately addresses. Additionally, biotin’s role in energy metabolism through pyruvate carboxylase could enhance ATP production in neurons, potentially protecting against the neurodegeneration that drives progressive disability.
A 2015 pilot study in 23 patients with progressive MS showed improvement in disability measures in 91% of patients treated with high-dose biotin, generating considerable excitement. The subsequent MS-SPI trial, a randomized, double-blind, placebo-controlled study of 154 patients, found that 12.6% of MD1003-treated patients achieved the primary endpoint of disability reversal at month 9, compared to 0% in the placebo group, a statistically significant difference45Tourbah, A., et al. “MD1003 (high-dose biotin) for the treatment of progressive multiple sclerosis: a randomised, double-blind, placebo-controlled study.” Multiple Sclerosis, 2016; 22(13): 1719-1731..
However, the definitive SPI2 trial, a larger phase 3 study of 642 patients across 90 centers in 13 countries, failed to confirm these findings. The proportion of patients showing disability improvement was 12% in the MD1003 group versus 9% in the placebo group, a difference that was not statistically significant (odds ratio 1.35, 95% CI 0.81-2.26). Furthermore, MD1003 caused significant laboratory test interference that complicated patient management throughout the trial46Cree, B.A.C., et al. “Safety and efficacy of MD1003 (high-dose biotin) in patients with progressive multiple sclerosis (SPI2): a randomised, double-blind, placebo-controlled, phase 3 trial.” Lancet Neurology, 2020; 19(12): 988-997..
An accompanying Lancet Neurology editorial was bluntly titled “High-dose biotin in multiple sclerosis: the end of the road,” concluding that the evidence did not support further development of high-dose biotin for MS, particularly given the lab test interference concerns47Motte, J., & Gold, R. “High-dose biotin in multiple sclerosis: the end of the road.” Lancet Neurology, 2020; 19(12): 965-966..
This trajectory, from promising pilot data through a positive phase 2 trial to a negative definitive trial, illustrates exactly why rigorous, adequately powered clinical trials are necessary and why preliminary results, no matter how encouraging, cannot be considered conclusive. The MS experience with biotin is a cautionary tale applicable to supplement science broadly.
Other Proposed and Emerging Applications
Peripheral Neuropathy
Peripheral neuropathy, particularly diabetic neuropathy, represents another area where biotin’s metabolic roles provide theoretical rationale for supplementation. Biotin’s involvement in nerve cell energy metabolism (through pyruvate carboxylase and the citric acid cycle) and in myelin synthesis (through acetyl-CoA carboxylase) suggests possible benefits for nerve function and repair. A small number of studies have reported improvements in neuropathic symptoms with high-dose biotin supplementation, but the evidence base remains too limited to support clinical recommendations48Koutsikos, D., et al. “Biotin for diabetic peripheral neuropathy.” Biomedicine & Pharmacotherapy, 1990; 44(10): 511-514..
Immune Function
Biotin deficiency impairs immune function, reducing natural killer cell activity and T-lymphocyte proliferation while increasing pro-inflammatory cytokine production through NF-κB activation. These observations have generated interest in whether biotin supplementation might enhance immune function in marginally deficient populations, such as older adults or individuals with chronic illness. However, the clinical evidence for immunomodulatory effects of biotin supplementation in non-deficient humans is essentially nonexistent49Kuroishi, T. “Regulation of immunological and inflammatory functions by biotin.” Canadian Journal of Physiology and Pharmacology, 2015; 93(12): 1091-1096..
Pregnancy and Fetal Development
Research by Mock and colleagues has demonstrated that marginal biotin deficiency is surprisingly common during pregnancy, affecting a substantial proportion of pregnant women based on sensitive biomarkers, and that biotin deficiency is profoundly teratogenic in animal models. In mice, biotin deficiency during pregnancy causes skeletal malformations (cleft palate, limb abnormalities) at rates comparable to those caused by folic acid deficiency. Whether marginal biotin deficiency in human pregnancy contributes to birth defects is unknown but represents a legitimate area of concern and active investigation50Mock, D.M. “Marginal biotin deficiency is common in normal human pregnancy and is highly teratogenic in mice.” Journal of Nutrition, 2009; 139(1): 154-157..
Most prenatal vitamins contain 30-300 mcg of biotin, which may or may not be sufficient to prevent marginal deficiency during pregnancy. The optimal biotin intake during pregnancy has not been established, and no large-scale trials have examined whether biotin supplementation beyond prenatal vitamin amounts reduces adverse pregnancy outcomes.
Dosing, Forms, and Practical Considerations
Supplement Doses vs. Physiological Requirements
The enormous gulf between biotin’s physiological requirement and the doses marketed in supplements demands careful examination. The Adequate Intake is 30 mcg/day. Common supplement doses range from 1,000 mcg (33× AI) to 10,000 mcg (333× AI), with some products containing 20,000 mcg or more. There is no established Tolerable Upper Intake Level (UL) for biotin, which is sometimes cited as evidence of safety, but the absence of a UL reflects insufficient data to set one, not a determination that any dose is safe51Institute of Medicine. “Dietary Reference Intakes for Thiamin, Riboflavin, Niacin, Vitamin B6, Folate, Vitamin B12, Pantothenic Acid, Biotin, and Choline.” National Academies Press, 1998..
Because biotin absorption follows saturable kinetics through the SMVT transporter, the proportion of biotin absorbed decreases as the dose increases. At a dose of 100 mcg, absorption efficiency is high (likely >50%). At 5,000 mcg, much of the dose passes through unabsorbed. At 10,000 mcg, you are paying for, and swallowing, large quantities of biotin that your body simply cannot use. This is true of most water-soluble vitamins at megadoses, but the sheer scale of the excess in typical biotin supplements makes the point particularly stark.
Evidence-Based Dosing Guidelines
Given the current evidence, dosing recommendations can be summarized as follows:
For general health maintenance: No supplementation is needed beyond what a balanced diet provides. If you choose to take a multivitamin, the biotin it contains (typically 30-300 mcg) is more than adequate.
For individuals at risk of deficiency (chronic anticonvulsant use, inflammatory bowel disease, chronic alcoholism, prolonged antibiotic use): 30-100 mcg/day from a supplement or multivitamin is a reasonable precautionary measure, though evidence-based dosing for these populations has not been established.
For brittle nail syndrome: 2,500 mcg/day for 3-6 months represents the dosing used in the limited (uncontrolled) studies showing benefit. Inform your healthcare provider about supplementation before any blood work.
For hair loss: There is no evidence-based dose because there is no evidence that biotin supplementation benefits hair growth in non-deficient individuals. If you choose to supplement despite this, be aware of the lab test interference risk at doses above 1,000 mcg.
For inherited biotin metabolism disorders (biotinidase deficiency, HCS deficiency): 10,000-30,000 mcg/day under medical supervision, with routine monitoring and awareness of lab test interference.
For diabetes/glucose metabolism: This is an area of active research. Doses of 2,000-9,000 mcg/day have been used in clinical studies, but supplementation should only occur under medical supervision given the potential for medication interactions and lab test interference.
Forms and Quality Considerations
Biotin is available as D-biotin (the naturally occurring, biologically active form) in supplements. Unlike some vitamins (vitamin E, for example), biotin does not have a synthetic racemic form that differs in biological activity, D-biotin is D-biotin regardless of manufacturing process. This means that product quality in biotin supplements primarily concerns accuracy of labeled potency, absence of contaminants, and dissolution characteristics rather than bioactive form differences.
Biotin supplements are available as standalone products, as components of B-complex formulations, and as ingredients in multivitamins and “beauty supplements.” The standalone products typically contain higher doses (1,000-10,000 mcg) while multivitamins contain lower, more physiologically appropriate amounts (30-300 mcg). Given the evidence, there is no scientific justification for choosing a high-dose standalone product over a standard multivitamin for most consumers.
As with all dietary supplements, third-party testing (USP Verified, NSF Certified for Sport, or ConsumerLab verified) provides reasonable assurance of label accuracy and purity. Products marketed specifically for hair growth at premium prices are delivering the same molecule available in far less expensive formulations.
Special Population Considerations
Vegetarians and Vegans
Unlike creatine, where vegetarians demonstrate consistently lower baseline levels and dramatically enhanced supplementation responses, biotin status in vegetarians does not appear to be significantly compromised. While the richest biotin sources (organ meats, eggs) are animal-derived, plant foods including nuts, legumes, whole grains, and some vegetables provide adequate biotin for most vegetarian diets. Vegans who consume varied diets including nuts, seeds, and legumes are similarly unlikely to develop deficiency. Intestinal bacterial synthesis may also contribute, though the magnitude of this contribution is debated52Said, H.M. “Biotin: biochemical, physiological and clinical aspects.” Subcellular Biochemistry, 2012; 56: 1-19..
Pregnant and Lactating Women
As noted above, marginal biotin depletion during pregnancy is surprisingly common based on sensitive biomarkers, even in women consuming adequate diets. The AI for pregnant women is 30 mcg/day (the same as for non-pregnant adults), though some researchers have argued this may be insufficient given the increased metabolic demands of pregnancy. Most prenatal vitamins contain biotin at levels that should prevent frank deficiency, but optimal intake during pregnancy has not been established. Women considering high-dose biotin supplementation during pregnancy should be aware that safety data at supraphysiological doses during pregnancy are limited.
Older Adults
Aging may affect biotin status through decreased dietary intake, reduced intestinal absorption, alterations in gut microbiome composition, and increased biotin catabolism from certain medications. However, frank biotin deficiency in otherwise healthy older adults is not well-documented, and the relevance of marginal depletion to age-related hair thinning, nail changes, or cognitive function remains speculative. The glucose metabolism research may be more relevant for older adults given the high prevalence of insulin resistance and type 2 diabetes in aging populations, but clinical evidence in this specific demographic is lacking.
Smokers
Smoking accelerates biotin catabolism, and smokers may require higher biotin intake to maintain adequate status. The StatPearls clinical reference notes that smokers may need increased doses when biotin supplementation is indicated. The clinical significance of this interaction for smokers not otherwise at risk of deficiency is unknown53Bistas, K.G., & Tadi, P. “Biotin.” In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing, 2023 (updated 2023 Jul 3)..
Drug Interactions
Beyond the lab test interference discussed above, biotin has several documented and theoretical drug interactions that merit awareness.
Anticonvulsants: Valproic acid, carbamazepine, phenytoin, and primidone can decrease biotin levels through various mechanisms including increased catabolism, decreased absorption, and inhibition of biotinidase. Patients on chronic anticonvulsant therapy represent one of the few populations where biotin supplementation (at modest doses of 30-100 mcg/day) may be rationally justified as a precautionary measure.
Antibiotics: Prolonged antibiotic use can reduce intestinal bacterial biotin synthesis, potentially contributing to marginal depletion in individuals with borderline dietary intake.
Isotretinoin: As discussed, isotretinoin reduces biotinidase activity and may cause biotin-responsive hair loss, one of the few scenarios where biotin supplementation for alopecia has some rational basis.
Pantothenic Acid (Vitamin B5): Because biotin and pantothenic acid share the SMVT transporter, very high doses of either vitamin could theoretically impair absorption of the other. This interaction is unlikely to be clinically significant at typical supplement doses but could be relevant at the megadoses sometimes used.
Alpha-Lipoic Acid: Also sharing the SMVT transporter, alpha-lipoic acid could compete with biotin for intestinal absorption at high doses. Patients taking both supplements might consider temporal separation of doses, though evidence for clinically significant interaction is limited.
Comprehensive Conclusion
Biotin is a genuinely essential nutrient with fascinating and complex biochemistry that extends well beyond its classical role as a carboxylase cofactor. Its emerging roles in gene regulation, epigenetic modification, glucose metabolism, and immune function represent legitimate frontiers of nutritional science that deserve continued investigation.
However, the current state of evidence does not support the primary use case driving the nearly $2 billion supplement market: hair growth in healthy individuals. The disconnect between marketing claims and research evidence is among the most extreme in the supplement industry. Not a single randomized controlled trial has demonstrated that biotin supplementation improves hair growth or quality in people without biotin deficiency. The evidence for nail health is slightly better but limited to uncontrolled studies in individuals with diagnosed brittle nail syndrome.
Meanwhile, the most clinically significant risk of biotin supplementation, interference with laboratory tests used to diagnose heart attacks, thyroid disease, pregnancy, cancer, and numerous other conditions, receives far less attention than it deserves. At least one death has been linked to biotin-induced lab test interference, and surveys indicate that the majority of biotin supplement users have never been warned about this risk.
The most promising legitimate research applications, glucose metabolism in diabetes, and the now-concluded MS investigation, involve pharmacological doses under medical supervision, a very different scenario from over-the-counter supplementation for cosmetic purposes.
For the evidence-based consumer, the practical conclusions are clear: a balanced diet provides adequate biotin for most people. If you wish to supplement, a standard multivitamin containing 30-300 mcg is sufficient and does not pose lab test interference risks. If you choose to take high-dose biotin for any reason, disclose this to every healthcare provider ordering blood work, and strongly consider discontinuing it before laboratory testing. And if your primary goal is improved hair or nail health, the evidence suggests your money would be better spent on addressing potential deficiencies in iron, zinc, or vitamin D, all of which have substantially stronger evidence bases for supporting hair and nail health than biotin does in non-deficient individuals.
This is the kind of analysis the supplement industry would prefer you never read. That is exactly why it needs to exist.
Generate Your Stack. Avoid Conflicts. Optimize Absorption.
Most supplement advice ignores timing, interactions, and dose-response curves. Smart Stack Builder doesn't. Get a personalized daily schedule with interaction flags and dosage guidance, built on the same evidence base as this article.
References
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
- 26
- 27
- 28
- 29
- 30
- 31
- 32
- 33
- 34
- 35
- 36
- 37
- 38
- 39
- 40
- 41
- 42
- 43
- 44
- 45
- 46
- 47
- 48
- 49
- 50
- 51
- 52
- 53
This article is part of our Supplements hub: A science-backed collection of ingredient research, clinical dosage reviews, and optimized stack insights.