Vitamin B6 (pyridoxine): what PLP does, supplementation evidence, and toxicity risks
Vitamin B6
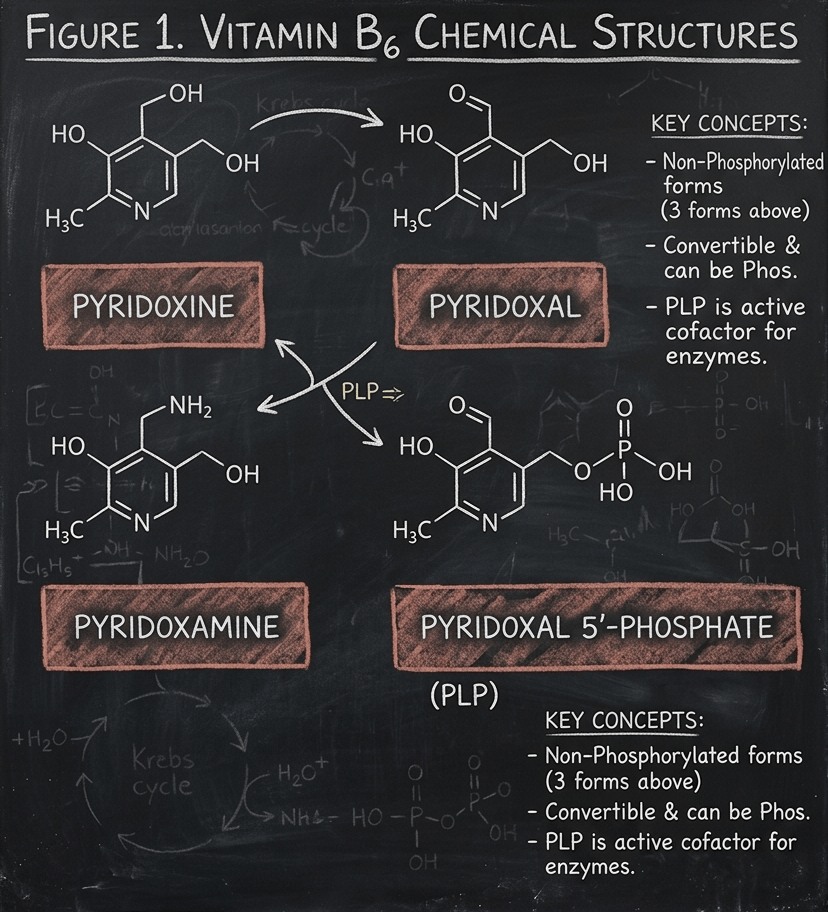
Vitamin B6 is not one molecule. It is a group of six related compounds: pyridoxine, pyridoxal, pyridoxamine, and their phosphorylated forms (pyridoxine 5′-phosphate, pyridoxal 5′-phosphate, and pyridoxamine 5′-phosphate). All six are interconvertible in the body, but the one that does the actual work is pyridoxal 5′-phosphate, or PLP. PLP is the coenzyme form, the version that sits in enzyme active sites and makes reactions happen.
And it makes a lot of reactions happen. The International Union of Biochemistry and Molecular Biology has catalogued over 140 PLP-dependent enzymatic activities, representing roughly 4% of all classified enzyme functions.1Percudani, R. and Peracchi, A. “A genomic overview of pyridoxal-phosphate-dependent enzymes.” EMBO Reports, 2003; 4(9): 850-854. That number keeps climbing as new enzyme databases expand, with some counts now exceeding 230 distinct catalytic functions across all organisms.2Du, Q., Wang, H., and Xie, J. “Thiamin (Vitamin B1) Biosynthesis and Regulation: A Rich Source of Antimicrobial Drug Targets?” International Journal of Biological Sciences, 2011; 7(1): 41-52. The scope of PLP’s involvement in human biochemistry is difficult to overstate: amino acid metabolism, neurotransmitter synthesis, hemoglobin production, immune function, glycogen mobilization, and one-carbon metabolism all depend on it.
The B vitamins overview on this site covers B6 in the context of the full B vitamin system. This article goes deeper into what PLP actually does, where B6 comes from, what the clinical evidence says about supplementation, and why the toxicity profile of this particular B vitamin deserves more attention than it typically receives.
A necessary disclaimer: If you have been diagnosed with a neurological condition, are pregnant, or are taking medications known to interfere with vitamin B6 metabolism (including isoniazid, certain anticonvulsants, or levodopa), work with a qualified medical professional. This article is educational. It is not a treatment plan, a diagnostic tool, or a substitute for clinical care.
What PLP does
PLP’s versatility comes from a single chemical trick. The molecule forms a covalent bond with amino acid substrates through a Schiff base linkage, creating an intermediate that stabilizes carbanionic (negatively charged carbon) species. This makes PLP an electron sink: it can absorb excess electron density from the substrate, which allows bonds that would otherwise be stable to break in controlled ways.3Eliot, A.C. and Kirsch, J.F. “Pyridoxal Phosphate Enzymes: Mechanistic, Structural, and Evolutionary Considerations.” Annual Review of Biochemistry, 2004; 73: 383-415. Different enzymes position the PLP-substrate complex in different orientations, and depending on which bond faces the pyridine ring, the reaction can proceed as a transamination, decarboxylation, racemization, elimination, or several other transformations. One cofactor, dozens of reaction types. The enzyme’s active site determines which reaction occurs; PLP provides the chemical machinery to make it possible.
This is not an abstract biochemistry detail. It explains why B6 deficiency produces such a wide range of symptoms: when the cofactor that participates in 4% of all enzymatic activity becomes scarce, the effects ripple through multiple systems simultaneously.
Amino acid metabolism
PLP is the cofactor for the aminotransferases (also called transaminases), the enzymes that shuttle amino groups between molecules. Alanine aminotransferase and aspartate aminotransferase, two of the most clinically measured enzymes in liver function panels, both require PLP. Without adequate PLP, amino acid interconversion stalls, affecting both the breakdown of dietary protein and the synthesis of nonessential amino acids.
PLP is also required for cystathionine β-synthase and cystathionine γ-lyase, the two enzymes of the transsulfuration pathway that convert homocysteine to cysteine. This connects B6 directly to homocysteine metabolism: when PLP is insufficient, the transsulfuration pathway slows and homocysteine accumulates. The B vitamins overview discusses the homocysteine connection in detail, but the short version is that B6, folate, and B12 collectively regulate homocysteine clearance through different mechanisms, and B6 handles the disposal route that produces cysteine, glutathione’s rate-limiting precursor.
Neurotransmitter synthesis
PLP is the cofactor for aromatic L-amino acid decarboxylase (AADC), the enzyme responsible for converting 5-hydroxytryptophan to serotonin and L-DOPA to dopamine.4Kennedy, D.O. “B Vitamins and the Brain: Mechanisms, Dose and Efficacy—A Review.” Nutrients, 2016; 8(2): 68. It is also required by glutamate decarboxylase, which produces GABA (the brain’s primary inhibitory neurotransmitter) from glutamate (the primary excitatory neurotransmitter). The balance between excitation and inhibition in the nervous system thus depends, at the enzymatic level, on PLP availability. This is why severe B6 deficiency can cause seizures, particularly in infants with genetic defects in PLP metabolism, and why the neurological symptoms of deficiency (irritability, depression, confusion) appear before most other signs.
Glycogen metabolism
PLP serves a structurally unusual role in glycogen phosphorylase, the enzyme that breaks down glycogen into glucose-1-phosphate for energy. In this case, PLP does not use its aldehyde group (the part involved in amino acid chemistry) but instead uses its phosphate group to facilitate acid-base catalysis.5Palm, D., Klein, H.W., Schinzel, R., Buehner, M., and Helmreich, E.J.M. “The role of pyridoxal 5′-phosphate in glycogen phosphorylase catalysis.” Biochemistry, 1990; 29(5): 1099-1107. Glycogen phosphorylase in muscle also serves as a storage reservoir for PLP; a substantial fraction of the body’s total PLP is sequestered in muscle tissue bound to this enzyme, which buffers circulating PLP levels but also means that muscle PLP does not respond quickly to dietary changes.
Immune function
B6’s role in immune function is real but primarily visible when status is low. PLP deficiency reduces lymphocyte proliferation, impairs T-cell mediated cytotoxicity, and decreases interleukin-2 production.6Meydani, S.N., Ribaya-Mercado, J.D., Russell, R.M., Sahyoun, N., Morrow, F.D., and Gershoff, S.N. “Vitamin B-6 deficiency impairs interleukin 2 production and lymphocyte proliferation in elderly adults.” American Journal of Clinical Nutrition, 1991; 53(5): 1275-1280. These effects are reversible with repletion. Plasma PLP also shows a consistent inverse association with inflammatory markers like C-reactive protein in population studies, though the direction of causation is not fully settled: inflammation itself appears to deplete PLP by increasing demand at sites of immune activity, so low PLP in the context of chronic disease may be partly a consequence of inflammation rather than a cause.7Ueland, P.M., McCann, A., Midttun, Ø., and Ulvik, A. “Inflammation, vitamin B6 and related pathways.” Molecular Aspects of Medicine, 2017; 53: 10-27.
One controlled feeding study in young women found that increasing B6 intake from 1.5 mg/day to 2.1 mg/day (slightly above the RDA) produced a 35% increase in lymphocyte proliferation. If that finding holds, it implies the immune system may be sensitive to B6 status even within the range conventionally considered adequate.8Kwak, H.K., Hansen, C.M., Leklem, J.E., Hardin, K., and Shultz, T.D. “Improved vitamin B-6 status is positively related to lymphocyte proliferation in young women consuming a controlled diet.” Journal of Nutrition, 2002; 132(11): 3308-3313.
The tryptophan-kynurenine pathway
PLP is a cofactor for several enzymes in the tryptophan-kynurenine pathway, which converts tryptophan into a range of metabolites with roles in immune regulation, NAD+ production, and neurotransmission. Kynureninase, the PLP-dependent enzyme that converts 3-hydroxykynurenine to 3-hydroxyanthranilic acid, is particularly sensitive to B6 status. When PLP is low, kynureninase activity drops and metabolism shifts toward producing xanthurenic acid instead. In fact, urinary xanthurenic acid excretion after a tryptophan load was one of the earliest functional biomarkers of B6 status, and it remains clinically relevant.9Leklem, J.E. “Quantitative aspects of tryptophan metabolism in humans and other species: a review.” American Journal of Clinical Nutrition, 1971; 24(6): 659-672.
This pathway matters beyond biomarker chemistry. Kynurenine pathway metabolites are immunomodulatory: they regulate T-cell proliferation, influence inflammatory cytokine production, and play a role in immune tolerance during pregnancy. The pathway is activated during inflammatory states, which increases PLP consumption and may partly explain why chronic inflammation depletes B6 status.
Absorption and metabolism
Dietary B6 exists in multiple forms. Animal-derived foods contain predominantly PLP and pyridoxamine 5′-phosphate. Plant-derived foods contain primarily pyridoxine and pyridoxine 5′-phosphate, sometimes in a glycosylated form called pyridoxine glucoside. This distinction matters for bioavailability: pyridoxine glucoside, which accounts for roughly 15% of B6 in a mixed diet, is only about 50% as bioavailable as other B6 forms.10Gregory, J.F. “Bioavailability of vitamin B-6.” European Journal of Clinical Nutrition, 1997; 51(Suppl 1): S43-S48. Overall bioavailability of B6 from a mixed diet is estimated at approximately 75%.
All phosphorylated forms are dephosphorylated by intestinal phosphatases before absorption. The non-phosphorylated vitamers (pyridoxine, pyridoxal, pyridoxamine) are absorbed in the jejunum primarily through passive diffusion, then transported to the liver via the portal circulation. In the liver, pyridoxal kinase phosphorylates them, and pyridoxine (pyridoxamine) 5′-phosphate oxidase converts PNP and PMP to PLP. The liver is the primary production site for plasma PLP, which circulates bound to albumin.11Institute of Medicine. Dietary Reference Intakes for Thiamin, Riboflavin, Niacin, Vitamin B6, Folate, Vitamin B12, Pantothenic Acid, Biotin, and Choline. Washington, DC: National Academies Press, 1998.
Excess B6 is metabolized to 4-pyridoxic acid, the primary urinary excretion product. This means B6 does not accumulate indefinitely in the way fat-soluble vitamins can, but it also means continuous dietary intake is necessary to maintain status. Plasma PLP has a half-life of roughly 25 days.
Dietary sources and requirements
Good dietary sources include poultry, fish (particularly tuna and salmon), beef liver, potatoes, starchy vegetables, chickpeas, bananas, and fortified cereals. The RDA for adults aged 19-50 is 1.3 mg/day for both men and women. Requirements increase modestly with age: 1.7 mg/day for men and 1.5 mg/day for women over 50. Pregnancy raises the requirement to 1.9 mg/day, and lactation to 2.0 mg/day.12Institute of Medicine. Dietary Reference Intakes for Thiamin, Riboflavin, Niacin, Vitamin B6, Folate, Vitamin B12, Pantothenic Acid, Biotin, and Choline. Washington, DC: National Academies Press, 1998.
The age-related increase in requirements is notable. Studies in older adults have consistently found that maintaining adequate plasma PLP requires higher intakes than in younger populations, likely due to changes in absorption efficiency and altered vitamin B6 metabolism. The RDA was set using plasma PLP of 20 nmol/L as the adequacy threshold, but some researchers have argued this cutoff is too low and that a target of 30 nmol/L or higher would better serve long-term health, particularly for immune function and cardiovascular risk reduction.
Median intake from food in the United States is approximately 2 mg/day for men and 1.4 mg/day for women. These numbers suggest most Americans meet the RDA, but NHANES data from 2003-2004 found that 24% of adults not taking B6-containing supplements had plasma PLP below 20 nmol/L.13Morris, M.S., Picciano, M.F., Jacques, P.F., and Selhub, J. “Plasma pyridoxal 5′-phosphate in the US population: the National Health and Nutrition Examination Survey, 2003-2004.” American Journal of Clinical Nutrition, 2008; 87(5): 1446-1454. Women, non-Hispanic Black adults, current smokers, and teenagers were disproportionately likely to have low status. B6 requirement scales with protein intake because so many PLP-dependent reactions involve amino acid metabolism, so high-protein diets increase the need for B6 even if they also tend to contain more of it.
The supplementation evidence
Nausea and vomiting in pregnancy
The strongest clinical application of B6 supplementation is for nausea and vomiting of pregnancy (NVP). Pyridoxine is one of only two FDA-approved pharmacological options for NVP (the other being the combination of doxylamine and pyridoxine, marketed as Diclegis/Diclectin). The American College of Obstetricians and Gynecologists recommends pyridoxine (10-25 mg, three or four times daily) as a first-line treatment.14ACOG Practice Bulletin No. 189. “Nausea and Vomiting of Pregnancy.” Obstetrics and Gynecology, 2018; 131(1): e15-e30.
The evidence base is modest but positive. A randomized, double-blind, placebo-controlled trial by Vutyavanich et al. found that 30 mg/day of pyridoxine significantly reduced nausea severity compared to placebo (p = 0.0008), with a trend toward fewer vomiting episodes that did not quite reach significance (p = 0.055).15Vutyavanich, T., Wongtra-ngan, S., and Ruangsri, R. “Pyridoxine for nausea and vomiting of pregnancy: a randomized, double-blind, placebo-controlled trial.” American Journal of Obstetrics and Gynecology, 1995; 193(3): 881-884. An earlier trial by Sahakian et al. found similar results, with the strongest benefit in patients with severe nausea.16Sahakian, V., Rouse, D., Sipes, S., Rose, N., and Niebyl, J. “Vitamin B6 is effective therapy for nausea and vomiting of pregnancy: a randomized, double-blind placebo-controlled study.” Obstetrics and Gynecology, 1991; 78(1): 33-36. A 2023 systematic review and meta-analysis of 18 studies confirmed that pyridoxine supplementation, both alone and in combination with other agents, produced beneficial effects for NVP.17Jayawardena, R., Majeed, S., Sooriyaarachchi, P., and Misra, A. “The effects of pyridoxine (vitamin B6) supplementation in nausea and vomiting during pregnancy: a systematic review and meta-analysis.” Archives of Gynecology and Obstetrics, 2023; 308(4): 1075-1085.
The mechanism of B6’s antiemetic effect is not fully understood. Given PLP’s role in serotonin synthesis and the kynurenine pathway, modulation of tryptophan metabolism is one plausible explanation, but this remains speculative.
Premenstrual syndrome
Vitamin B6 has been used to treat premenstrual syndrome (PMS) for decades, and the evidence is suggestive but not strong. A systematic review by Wyatt et al. in the BMJ found a pooled odds ratio of 2.32 (95% CI: 1.95-2.54) in favor of B6 for overall premenstrual symptoms across nine randomized trials, with a similar effect for depressive symptoms specifically (OR 2.12, 95% CI: 1.80-2.48).18Wyatt, K.M., Dimmock, P.W., Jones, P.W., and Shaughn O’Brien, P.M. “Efficacy of vitamin B-6 in the treatment of premenstrual syndrome: systematic review.” BMJ, 1999; 318(7195): 1375-1381. The authors concluded that B6 was likely more effective than placebo but emphasized that the quality of the included studies was generally poor.
A more recent double-blind RCT found that 80 mg/day of pyridoxine over three menstrual cycles produced significant reductions in a range of PMS symptoms, with the strongest effects on anxiety.19Kashanian, M., Mazinani, R., and Jalalmanesh, S. “Pyridoxine (vitamin B6) therapy for premenstrual syndrome.” International Journal of Gynecology and Obstetrics, 2007; 96(1): 43-44. The rationale for B6’s effect on PMS typically invokes its role in serotonin and dopamine synthesis, though the precise mechanism has not been established.
The evidence is enough to consider B6 a plausible option for PMS management, particularly for mood-related symptoms, but it is not enough to make a confident recommendation. Doses in most positive trials ranged from 50-100 mg/day, which brings the toxicity profile into play (discussed below).
Cardiovascular disease and homocysteine
B6 supplementation reliably lowers homocysteine levels, particularly when combined with folate and B12. The question is whether this translates into cardiovascular benefit. The answer, based on the available trial data, is mostly no. The major randomized trials of B vitamin supplementation for cardiovascular disease prevention (HOPE-2, VISP, NORVIT) found that while homocysteine levels decreased, cardiovascular event rates did not improve significantly in populations with existing cardiovascular disease.20Martí-Carvajal, A.J., Solà, I., Lathyris, D., and Dayer, M. “Homocysteine-lowering interventions for preventing cardiovascular events.” Cochrane Database of Systematic Reviews, 2017; 8: CD006612.
This disconnect is discussed in the B vitamins overview. The practical takeaway is that while B6 contributes to homocysteine clearance and maintaining adequate B6 status is important for one-carbon metabolism, supplementing B6 to lower homocysteine as a cardiovascular intervention is not supported by the trial evidence.
Cognitive decline
Observational studies have found associations between low B6 status and cognitive decline in older adults. Given B6’s role in neurotransmitter synthesis, this is biologically plausible. However, randomized trials of B vitamin supplementation for cognitive outcomes have been inconsistent, and it is difficult to isolate B6’s contribution because most trials used combined B vitamin interventions (typically B6 + B12 + folate). There is no compelling evidence that B6 supplementation alone prevents or slows cognitive decline in people with adequate B6 status.21Ford, A.H. and Almeida, O.P. “Effect of vitamin B supplementation on cognitive function in the elderly: a systematic review and meta-analysis.” Drugs and Aging, 2019; 36(5): 419-434.
Toxicity: the B vitamin that can hurt you
B6 is the one B vitamin with a well-established toxicity profile, and the story is more complicated than most supplement labels suggest.
The classical teaching is that sensory neuropathy (numbness, tingling, burning, and loss of proprioception in the hands and feet) develops at chronic doses above 1,000 mg/day, and that the IOM’s tolerable upper intake level of 100 mg/day provides an adequate safety margin. That is partly true but increasingly recognized as incomplete.
The neuropathy is primarily sensory and involves the dorsal root ganglia. It is dose-dependent, with higher doses producing more severe symptoms, and duration-dependent, with the time to symptom onset inversely proportional to the daily dose. At very high doses (2,000 mg/day or above), symptoms can develop in weeks and may be irreversible. At lower doses, onset may take months or years, and symptoms typically reverse after discontinuation, although a phenomenon called “coasting” can cause temporary worsening before improvement begins.22Gdynia, H.J., Müller, T., Sperfeld, A.D., Kühnlein, P., Otto, M., Kassubek, J., and Ludolph, A.C. “Severe sensorimotor neuropathy after intake of highest dosages of vitamin B6.” Neuromuscular Disorders, 2008; 18(2): 156-158.
What has changed in recent years is the recognition that neuropathy can occur at doses well below the traditional 100 mg/day threshold. The Australian Therapeutic Goods Administration reviewed adverse event reports and found cases of peripheral neuropathy at daily doses below 50 mg, including in patients taking multiple supplements containing B6 without realizing their total intake.23Therapeutic Goods Administration. “Peripheral neuropathy with supplementary vitamin B6 (pyridoxine).” Safety Update, October 2022. The TGA responded by requiring warning labels on any product providing more than 10 mg/day of B6 and lowering the maximum permitted daily dose in supplements from 200 mg to 100 mg. The European Food Safety Authority set an adult upper limit of 12 mg/day in 2023, dramatically lower than the US threshold of 100 mg/day. The UK Expert Group on Vitamins and Minerals had previously flagged caution above 10 mg/day for long-term use.
The mechanism of pyridoxine neurotoxicity is still debated, but the leading hypothesis involves a paradoxical effect: at high concentrations, pyridoxine inhibits pyridoxal kinase, the very enzyme that converts it to the active PLP form. This means that high-dose pyridoxine supplementation can actually reduce functional PLP availability in peripheral tissues, creating a local B6 deficiency even as circulating pyridoxine levels are elevated.24Vrolijk, M.F., Opperhuizen, A., Jansen, E.H.J.M., Hageman, G.J., Bast, A., and Haenen, G.R.M.M. “The vitamin B6 paradox: Supplementation with high concentrations of pyridoxine leads to decreased vitamin B6 function.” Toxicology In Vitro, 2017; 44: 206-212. Because the blood-brain barrier is relatively impermeable to pyridoxine, this inhibitory effect is confined to peripheral tissues, which may explain why the neuropathy is predominantly peripheral rather than central.
This “vitamin B6 paradox” has practical implications. Some researchers and clinicians have suggested that supplementing with pyridoxal 5′-phosphate (the active form, sometimes sold as P5P) rather than pyridoxine might reduce the risk of neuropathy because it bypasses the pyridoxal kinase step. The logic is sound, but clinical evidence confirming a lower risk with PLP supplementation is limited, and regulatory bodies have not yet differentiated between B6 forms in their upper limit recommendations.
The key takeaway: B6 toxicity is not just a concern at megadoses. Individual susceptibility varies, there is no established safe threshold for long-term supplementation, and people often consume B6 from multiple sources without realizing it. Magnesium supplements, zinc supplements, B-complex formulations, and multivitamins frequently contain B6. Checking cumulative intake across all supplements is worth the effort.
Who benefits from supplementation
Most people eating a varied diet that includes animal products get enough B6 without supplementing. The populations with a genuine case for targeted supplementation include:
Pregnant women experiencing nausea and vomiting have the strongest evidence-based reason to supplement, with pyridoxine at 10-25 mg three to four times daily recommended as a first-line intervention by ACOG. Pregnancy also increases the RDA for B6 to 1.9 mg/day, so a modest supplement may be warranted even without NVP symptoms.
Older adults are at increased risk for inadequate B6 status due to reduced absorption and altered metabolism. The IOM increased the RDA for adults over 50 (1.7 mg/day for men, 1.5 mg/day for women) but some evidence suggests even these levels may be insufficient for optimal immune function.
People taking medications that deplete B6, including isoniazid (tuberculosis treatment), cycloserine, penicillamine, levodopa, certain anticonvulsants (valproic acid, carbamazepine, phenytoin), and hydralazine, may need targeted supplementation. Isoniazid is the most clinically significant interaction; pyridoxine co-administration at 10-25 mg/day is standard practice during isoniazid therapy to prevent neuropathy.25Snider, D.E. “Pyridoxine supplementation during isoniazid therapy.” Tubercle, 1980; 61(4): 191-196.
People with chronic inflammatory conditions, including rheumatoid arthritis, inflammatory bowel disease, and celiac disease, tend to have lower plasma PLP concentrations. Whether this reflects increased consumption of PLP at sites of inflammation or impaired absorption depends on the condition, but monitoring B6 status and supplementing if deficient is reasonable.
People on oral contraceptives may have reduced PLP levels, though the clinical significance of this finding is debated. The mechanism appears related to estrogen’s effect on tryptophan metabolism rather than true B6 depletion, but some researchers recommend B6 supplementation for women on hormonal contraceptives, particularly those planning future pregnancy.
Heavy alcohol users are at risk for B6 depletion because alcohol’s primary metabolite, acetaldehyde, displaces PLP from its protein binding sites and accelerates its degradation.
For the general population with adequate dietary intake, a low-dose B6 supplement (under 10 mg/day) carries minimal risk and may provide marginal benefit as part of a B-complex, but the expected return on supplementation is small.
Conclusion
Vitamin B6 occupies an unusual position among the B vitamins. Its active form, PLP, participates in a wider range of enzymatic reactions than any other B vitamin cofactor, touching amino acid metabolism, neurotransmitter production, immune regulation, glycogen mobilization, and the tryptophan-kynurenine pathway. Despite this biochemical importance, the supplementation evidence for B6 in non-deficient populations is limited to a few specific applications: NVP in pregnancy (well-supported), PMS symptom relief (suggestive but based on weak evidence), and maintenance of immune function in populations at risk for marginal deficiency (plausible but not conclusively demonstrated in supplementation trials).
The toxicity story is the part that deserves the most attention. B6 is the only water-soluble vitamin with a well-documented capacity to cause nerve damage at supplemental doses, and the safety threshold appears lower than previously recognized. The gap between the US upper limit (100 mg/day) and the European upper limit (12 mg/day) reflects genuine scientific uncertainty about where the safe boundary lies. For anyone supplementing B6, keeping daily intake below 10 mg for long-term use is the most conservative approach, checking total intake across all supplements is important, and any symptoms of tingling or numbness in the extremities should prompt immediate discontinuation and medical evaluation.
Generate Your Stack. Avoid Conflicts. Optimize Absorption.
Most supplement advice ignores timing, interactions, and dose-response curves. Smart Stack Builder doesn't. Get a personalized daily schedule with interaction flags and dosage guidance, built on the same evidence base as this article.
References
- 1
- 2
- 3
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11
- 12
- 13
- 14
- 15
- 16
- 17
- 18
- 19
- 20
- 21
- 22
- 23
- 24
- 25
This article is part of our Supplements hub: A science-backed collection of ingredient research, clinical dosage reviews, and optimized stack insights.